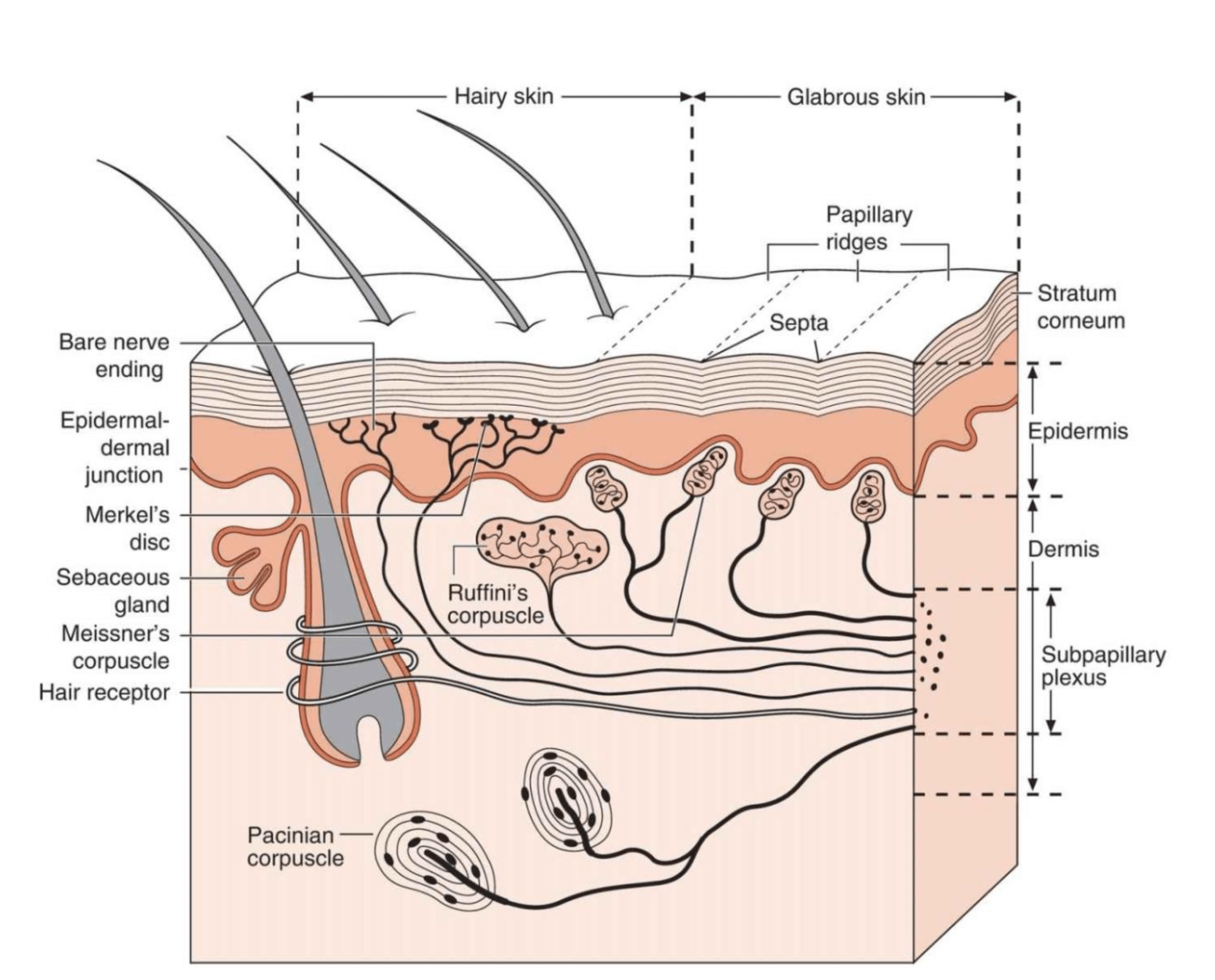
- What Are Tactile Cues and How Do They Help Recovery? - 28 March 2026
- Parsonage-Turner Syndrome and COVID-19: What the Research Shows - 28 March 2026
- Managing Pain in the Acute Phase of Parsonage-Turner Syndrome - 28 March 2026
Here’s something that most people recovering from Parsonage-Turner syndrome don’t get told. The nerve damage in your arm isn’t the whole story. There’s a second problem happening further up the chain, inside your brain, and if nobody addresses it then recovery stalls no matter how much physiotherapy you throw at the muscles. We’ve seen this pattern over and over, someone whose nerve is technically healing but whose arm still doesn’t work properly. The missing piece is what’s happening at the cortical level.
This article is part of our comprehensive guide to Parsonage-Turner syndrome.
So that’s what this article is about. We’re going to look at what actually happens in your brain after PTS, why it matters for recovery, and how sensory mapping can help put things right. If you’ve already read our full PTS guide, this goes deeper into the neuroscience behind our approach. And if you haven’t, that’s a good place to start for the broader picture.
Fair warning, this one gets a bit nerdy. But we think understanding what’s going on in your brain is genuinely useful when it comes to recovery, because it explains why certain rehabilitation approaches work and others fall short.
This article covers:
What Actually Happens in Your Brain After PTS
When the brachial plexus gets damaged by Parsonage-Turner syndrome, the obvious effects are the ones you can see and feel. Pain, weakness, muscle wasting. But there’s a parallel process happening in the brain that’s just as significant, even though you can’t feel it directly.
Your brain maintains detailed maps of your body. The somatosensory cortex has specific regions dedicated to processing sensory information from your hand, forearm and shoulder, all fed by the brachial plexus. When the nerve signals from your arm suddenly change or stop entirely, those maps don’t just sit there waiting for the nerves to grow back. They start to reorganise [1].
This reorganisation is called cortical plasticity, and in other contexts it’s a good thing. It’s how your brain learns new skills and recovers from strokes. But after peripheral nerve injury, the plasticity that occurs is often maladaptive. The brain’s maps become distorted, neighbouring regions encroach on the territory that used to belong to your arm and the result is a cortical representation that no longer matches your actual limb [2].
Think of it like a radio that’s lost its station. The signal from your brachial plexus has been disrupted, so the brain starts picking up interference from other channels. After weeks or months of this, the brain’s “tuning” for your arm becomes genuinely scrambled. It’s not just a case of waiting for the signal to come back, the receiver itself has changed.
The Research: What fMRI Studies Tell Us
This isn’t just theoretical. There’s actual imaging data showing exactly what goes wrong in the brain after neuralgic amyotrophy.
A particularly important study by Lustenhouwer and colleagues in 2022 used functional MRI to examine 39 patients with neuralgic amyotrophy [3]. What they found was striking, decreased cerebral activity in visuomotor areas, specifically the extrastriate cortex and parieto-occipital sulcus. These are regions involved in planning movements based on what you see and in coordinating hand-eye tasks.
But here’s the really interesting part. The decrease in brain activity was directly correlated with persistent pain. Patients with more persistent pain showed less activity in these visuomotor areas, with a correlation of r=-0.45 (p=0.004) [3]. That’s a meaningful relationship, suggesting the brain changes aren’t just a side effect of PTS, they’re actively contributing to ongoing symptoms.
Why does this matter practically? Because even after the peripheral nerve starts to regenerate, the brain may not be ready to use those signals properly. You could have a perfectly healed nerve but still struggle with movement and pain because the cortical maps haven’t been restored. If your rehabilitation is only focused on the muscles, it’s missing half the problem.
However, the Lustenhouwer study also points toward a solution. If visuomotor strategies can be incorporated into rehabilitation targeting those underactive brain areas, outcomes could improve. This is where mirror therapy and sensory re-education come in, which we’ll get to shortly.
Maladaptive Plasticity: When Your Brain Works Against You
Maladaptive plasticity is one of those concepts that sounds intimidating but is actually quite straightforward once you break it down. Your brain is constantly reorganising itself based on the information it receives. When it comes to nerve injuries like PTS, that information changes dramatically. The signals from your shoulder and arm become unreliable, reduced, or absent altogether, and the brain adapts to this new reality.
The problem is that the adaptations aren’t helpful. Motor planning goes awry because the brain’s map of your arm no longer matches the actual anatomy. Sensory processing becomes distorted as cortical regions get partially taken over by neighbouring areas. Compensatory movement patterns develop, things like shoulder hiking and trunk shifting, which the brain starts to treat as normal.
Li and colleagues found that cortical plasticity and peripheral nerve regeneration are actually interlinked processes [4]. The brain doesn’t passively wait for the nerve to regrow, the state of the cortical maps actively influences how well regenerating nerve fibres find their targets. If the cortical maps have become significantly disordered, they can impede nerve recovery. It’s a feedback loop, and not a kind one.
For those with hypermobility who’ve dealt with chronic pain or recurrent issues like wrist instability and hypermobile elbows, this concept of the brain amplifying or perpetuating problems will sound familiar. The brain’s role in maintaining symptoms is something we talk about a lot in our work, and PTS is perhaps one of the clearest examples of it in action.
There’s a bit of a tangent here but it’s something worth mentioning. I find it fascinating that the same neural plasticity that allows a musician to develop extraordinary finger dexterity is the same mechanism that, after nerve injury, can work against recovery. The brain’s ability to change is neither good nor bad on its own, it depends entirely on the signals it’s receiving. And that’s actually the whole basis for why sensory mapping works, you’re giving the brain better signals to reorganise around.
Why Traditional Rehab Often Falls Short
So here’s the question nobody seems to ask often enough: if PTS involves significant brain changes, why does most rehabilitation focus almost entirely on the muscles?
Traditional physiotherapy for Parsonage Turner syndrome typically involves range of motion exercises, progressive strengthening, and maybe some electrical stimulation. Those things aren’t wrong, they’re necessary. But they’re incomplete because they don’t address the cortical component.
It’s like trying to fix a software problem by replacing the hardware. You might get some improvement, the stronger muscles can compensate to a degree, but you’re not solving the underlying issue. The brain still has disordered maps, motor planning is still disrupted and sensory integration is still off. This is why so many people with PTS report that they’ve “done all the exercises” but still can’t use their arm normally. The exercises weren’t wrong, they were just insufficient.
The statistics back this up. Despite nerve recovery occurring in the majority of PTS cases, up to 70% don’t achieve complete return of motor function and around 60% are left with residual neuropathic pain [6]. Those numbers suggest something beyond peripheral nerve healing is needed. When it comes to rehabilitation, we think that something is cortical reorganisation.
A major review in Frontiers in Neurology confirmed that cortical remodelling theory underpins modern brachial plexus rehabilitation approaches. The evidence base is growing for interventions that target the brain directly, not just the muscles. For those with hypermobility who are used to exercise being about more than just strength, this neurology-first approach will sound very familiar.
Sensory Mapping: What It Is and How It Works
Right, so if the problem is partly in the brain, what do we actually do about it? This is where sensory mapping comes in, and it’s one of the things that makes our approach different.
Sensory mapping, or sensory re-education as the research literature calls it, involves systematically providing the brain with structured sensory input to rebuild accurate cortical representations of the affected limb. Florence and colleagues demonstrated in 2001 that sensory enrichment could restore cortical maps after peripheral nerve damage [1]. What’s changed since is our understanding of how and why it works.
Philip and Zink published a scoping review in 2020 identifying seven rehabilitative interventions based on cortical plasticity principles for upper extremity peripheral nerve injuries [2]. These include:
- Traditional sensory re-education (tactile discrimination exercises)
- Activity-based sensory re-education (functional tasks with sensory focus)
- Mirror therapy
- Mental motor imagery
- Cross-modal sensory substitution
- Action observation with peripheral nerve stimulation
- Selective deafferentation techniques
What connects all of these is that they work at the cortical level. They’re not trying to strengthen a weak deltoid or stretch a stiff shoulder, they’re providing the brain with information that helps it recalibrate its maps. Some work through visual input, some through tactile input, some through imagined movement. But the target is always the brain [2].
Mirror therapy deserves special attention here. Chen and colleagues in 2022 studied it after peripheral nerve repair and found greater cortical activation compared to classical sensory relearning [8]. Patients showed better finger and manual dexterity and brain imaging revealed greater activation in multimodal association cortices. It was doing more for the brain than standard approaches, and that translated into better function.
For anyone who has dealt with CRPS, you’ll recognise this approach. Mirror therapy has been used in complex regional pain syndrome for years and the overlap between CRPS and PTS in terms of cortical reorganisation has informed how we work.
Reversing Maladaptive Plasticity: It Can Be Done
One of the most encouraging pieces of research comes from a 2019 study in Nature Communications that examined closed-loop vagus nerve stimulation after peripheral nerve damage [9]. The researchers found that reversing maladaptive central plasticity was sufficient to improve both motor and sensory function. They didn’t repair the nerve better or strengthen the muscles more. They corrected the brain’s response to the injury, and function improved.
Vagus nerve stimulation isn’t widely available for PTS rehabilitation. But the principle it demonstrates is what matters. If you can get the brain to reorganise its maps more accurately, recovery improves even without doing anything additional to the nerve or muscles. That’s what underpins sensory mapping, motor imagery, mirror therapy and the other cortical-focused approaches we use.
However, it’s worth being honest about the limitations. Most cortical plasticity research comes from studies on median and ulnar nerve injuries, not specifically brachial plexus injuries like PTS. The brachial plexus is more complex, involving multiple nerves, and the cortical reorganisation is likely more extensive. We’re extrapolating from related evidence, and while the logic is sound, more PTS-specific research would be welcome.
Our Approach: How We Use This at The Fibro Guy
How does all of this translate into what we actually do with people who come to us with Parsonage-Turner syndrome?
Our approach has always been rooted in the idea that the nervous system is the key, whether we’re working with those with hypermobility, chronic pain conditions, or peripheral nerve injuries. When it comes to PTS, we use a combination of tactile cues, progressive motor learning and sensory re-education that targets cortical reorganisation directly.
Tactile Cues for Somatosensory Rebuilding
We use external feedback through touch, pressure and different textures to give the brain structured sensory input about the affected arm and shoulder. This isn’t random massage or general “touching the area”. It’s specific, graded tactile stimulation designed to help the somatosensory cortex rebuild its representation of the limb. The same approach we use for core stability work in hypermobility translates directly, the underlying principle is identical: give the brain better information and it produces better output.
Things like KT tape and compression garments play a role here too. They provide constant proprioceptive feedback to the affected area, essentially giving the brain a low-level stream of information about where the arm is in space. For those with hypermobility who already have reduced proprioception, that extra input is even more valuable.
Progressive Motor Learning
We don’t just ask people to “strengthen” their shoulder. Strengthening implies the muscle already knows what to do and simply needs more capacity. When cortical maps are disordered, motor planning itself is compromised. So we use progressive motor learning, reteaching the brain how to plan and execute movements from the ground up.
This might start with very simple scapular control tasks and progress through to more complex functional movements, not unlike our approach to shoulder blade rehabilitation or motor retraining in the lower limb, but adapted for the neurological demands of PTS. The progression follows the logic of cortical reorganisation, easier patterns first, then gradually increasing complexity as the brain’s maps improve. We’ve written more about exercise progressions in our PTS exercise and rehabilitation article.
Addressing Fear and the Emotional Component
We’d be doing you a disservice if we didn’t mention this. After the kind of pain that PTS delivers, fear of movement is completely understandable. But fear has its own effects on cortical processing, it heightens threat detection, amplifies pain signalling and makes the brain less willing to engage the motor patterns needed for recovery. The anxiety that accompanies a PTS diagnosis can become its own barrier if it isn’t addressed.
Graded exposure, education and building genuine confidence in the affected limb are all part of what we do. This connects back to cortical reorganisation, as confidence and positive movement experiences help the brain recalibrate its threat assessment of the limb.
What This Means for Your Recovery
If you’re in the middle of recovering from PTS, or if you feel like your recovery has plateaued, here’s what all of this means in practical terms.
First, if your current rehabilitation is purely exercise-based, focused only on strength and range of motion, it’s probably not enough. That doesn’t mean stop those exercises. It means you should be doing more alongside them, specifically things that target the brain’s representation of your arm. Mirror therapy is something you can explore with a physiotherapist. Sensory re-education exercises involving different textures, temperatures and tactile discrimination tasks are straightforward to incorporate. Mental motor imagery, where you vividly imagine performing movements with your affected arm, has evidence behind it and costs nothing [2].
Second, don’t panic about the brain changes. Cortical reorganisation is happening, yes, but it’s also reversible. The research shows that with the right inputs the brain can recalibrate its maps. That’s the whole point of plasticity, it works both ways [9]. When it comes to recovery from neuralgic amyotrophy, the brain’s ability to change is what makes full recovery possible.
Third, pace yourself. Cortical reorganisation takes time, just like nerve regeneration. Pushing too hard too fast doesn’t speed up the brain changes, it can reinforce compensatory patterns that you’re trying to undo. The phases of PTS recovery exist for a reason and each phase has different neurological demands.
And finally, if you’re dealing with persistent symptoms despite apparently good nerve recovery, this might explain why. It’s not that you’re not trying hard enough, it’s that the brain component hasn’t been addressed. The medical trauma of being told nothing more can be done when there’s a whole dimension of rehabilitation that hasn’t been tried, that’s something we see far too often.
The Bigger Picture: PTS and Connected Systems
One thing we should mention before moving to the FAQ. The brain changes after PTS don’t exist in isolation, they connect to other systems that are often already under strain.
When it comes to breathing, the muscles of the shoulder girdle overlap significantly with the accessory breathing muscles. If those muscles are compromised by PTS and the brain’s motor planning for the area is disrupted, breathing mechanics can be affected too. We’ve seen people develop compensatory breathing patterns during PTS that persist after the shoulder muscles have recovered, because the cortical maps governing those movements haven’t been corrected.
Likewise, altered shoulder mechanics can lead to knock-on issues elsewhere. Rib subluxations from changed movement patterns, postural adaptations that start to resemble scoliosis patterns, coat hanger pain from altered upper back mechanics, these are all things we keep an eye on. For those already dealing with neurological processing issues related to hypermobility, PTS adds another layer that needs careful management.
Frequently Asked Questions
Does everyone with PTS experience brain changes?
Yes, to varying degrees. Any disruption to peripheral nerve signalling will cause some cortical reorganisation, the brain simply responds to the change in input. However the extent varies depending on which nerves are affected, the severity of damage, and how long the disruption lasts [3]. Some people have relatively minor cortical changes that resolve naturally, others have more significant reorganisation that needs active rehabilitation to correct.
Can I do sensory mapping exercises at home?
Some sensory re-education exercises can be done at home. Texture discrimination tasks, where you practise identifying different materials by touch with your affected hand, is one example. Mirror therapy can be set up at home with guidance. However, we’d recommend working with a therapist who understands the cortical component of PTS before starting, because the exercises need to be appropriately graded for your current phase of recovery. Our exercise article covers the principles in more detail.
How long does it take for the brain to reorganise after PTS?
There’s no simple answer to this. Cortical reorganisation begins almost immediately after nerve injury and continues throughout recovery. The maladaptive changes can start developing within days to weeks. Reversing those changes with targeted rehabilitation is slower, typically months rather than weeks, and it broadly follows the timeline of nerve regeneration. Most people see meaningful improvements within 3 to 6 months, but the full process can take longer.
Is this the same as what happens in phantom limb pain?
There are similarities. Phantom limb pain involves cortical reorganisation after limb loss, and the mechanisms share common ground with what happens after brachial plexus injury. In both cases the brain’s maps become distorted when expected sensory input stops arriving. However, PTS is different because the nerve damage is usually temporary and the limb is still present, which gives rehabilitation more to work with. The brain can receive actual sensory input from the affected limb, it just needs help interpreting it correctly again.
My therapist only focuses on strength exercises. Should I be concerned?
Not concerned exactly, because strengthening is still important for PTS rehabilitation. But if your recovery has stalled or you feel like something is missing, it’s worth asking about sensory re-education and cortical-focused approaches. Not all physiotherapists are familiar with these methods for PTS specifically. Our article on PTS diagnosis includes suggestions for what to discuss with your healthcare team, and our living with PTS guide covers finding appropriate support.
Where to Go From Here
Understanding the brain’s role in PTS recovery changes how you think about rehabilitation. It’s not just about waiting for the nerve to heal and doing your exercises, it’s about actively helping the brain rebuild its maps so that when nerve signals do return, the brain knows what to do with them.
If you want to explore this further, our PTS hub page covers everything from causes to treatment, including how conditions like EDS flare-ups can complicate the picture. For practical rehabilitation guidance, see our PTS exercise article. And if you’re still in the early stages, our articles on acute pain management and the phases of recovery will help you understand where you are in the process.
We’re here if you need us. Whether you’re at the start of this or months in feeling frustrated, understanding the brain component is often the thing that makes the difference.
– The Fibro Guy Team –
Where to Go From Here
If you’re working through recovery from Parsonage-Turner syndrome, the principles we use in our studios — neuron-first rehab, sensory mapping, graded loading — are the same ones that underpin our Hypermobility 101 course. It covers the frameworks for rebuilding joint control and proprioception that are directly relevant to PTS recovery. Have a look through the full course library for everything we offer.