Please click below if you prefer to listen to this article on Parsonage-Turner syndrome.
I first wrote this article on Parsonage-Turner syndrome way back in 2017, and in the years since, I have worked with more people with PTS. So, I wanted to revisit this article to add more information for people regarding exercise and rehab for those living with PTS.
This article covers:
ToggleWhat is Parsonage-Turner syndrome?
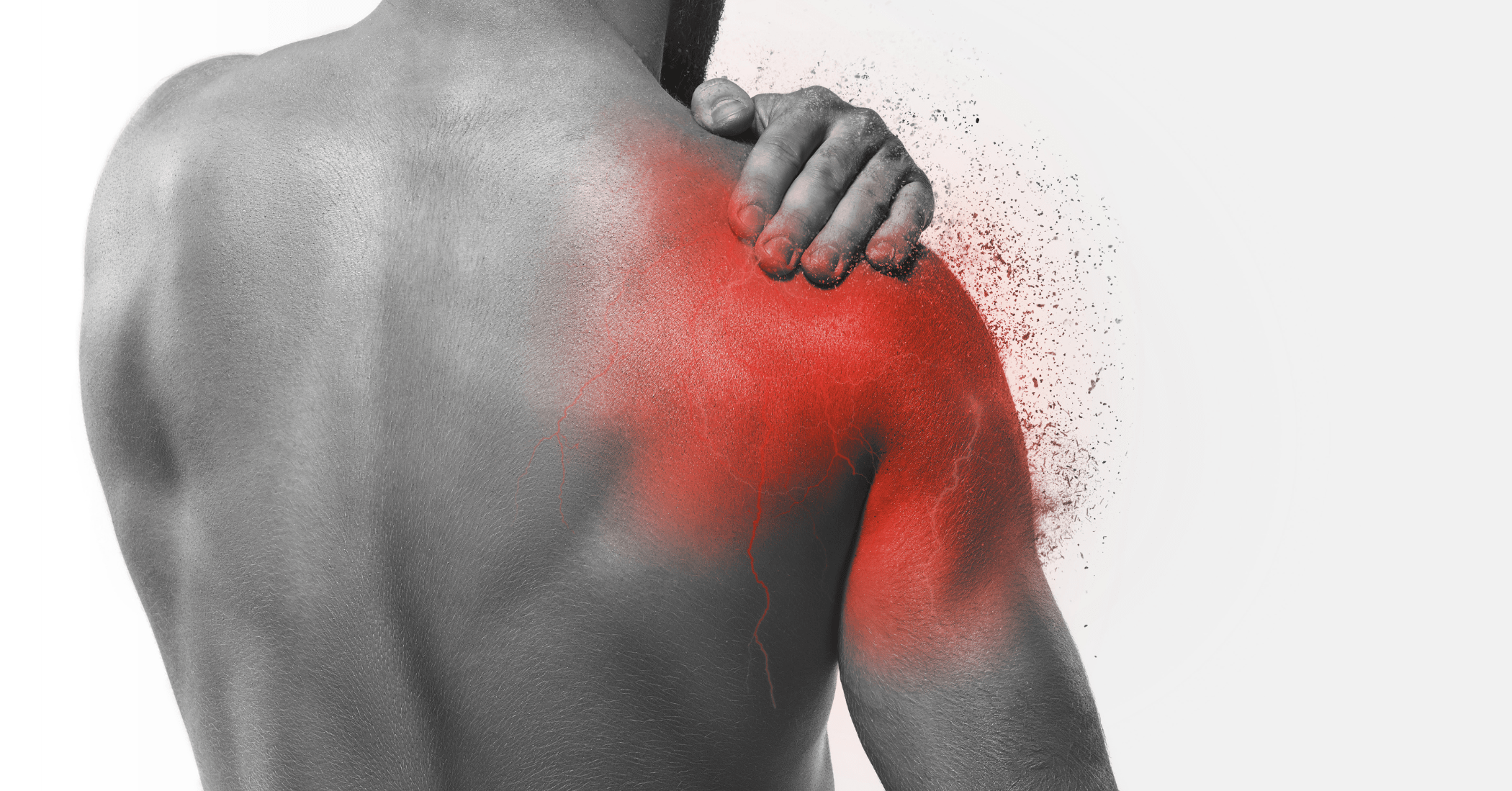
Parsonage-Turner syndrome (PTS), also known as Neuralgic Amyotrophy, is an uncommon neurological disorder characterised by a rapid onset of severe pain in the shoulder and arm. This acute phase may last a few hours to a few weeks and is followed by wasting and weakness of the muscles (amyotrophy) in their affected areas. For those with PTS, daily tasks that most of us take for granted can become increasingly difficult over time, as weakness, atrophy, and pain interfere with everyday tasks.
Parsonage-Turner syndrome mainly involves the brachial plexus, the network of nerves that extend from the spine through the neck, into each armpit, and down the arms. These nerves control movements and sensations in the shoulders, arms, elbows, hands, and wrists. However, other nerves in the arm or leg can also be involved.
What causes PTS?
Whilst not much is known about the causes of Parsonage-Turner syndrome, researchers suspect that most cases are due to an autoimmune response following exposure to an illness or environmental factor.
Now, back in 2017, when I first met Alison (you will meet her soon), I was astounded by the sheer lack of research on PTS, with Pubmed yielding around 1,700 articles on the topic (and 1,783 for Neuralgic amyotrophy). Sadly, in 2024, when I looked again, that number has only risen to 1,996 (and 2,096 for Neuralgic amyotrophy)
However, as you will see from the image below, there has been a recent uptick in research into PTS. Now, I wonder why this might be.
If only something were health-destroying around 2019: oh, Covid-19!
FAQs on Parsonage-Turner Syndrome
What is the pain pattern of Parsonage-Turner syndrome?
Parsonage-Turner syndrome typically begins with a sudden, intense pain in the shoulder and upper arm. This acute pain can last from a few hours to several weeks, often followed by muscle weakness and wasting in the affected areas. As the initial severe pain subsides, it may be replaced by a persistent, dull ache and noticeable difficulty in everyday tasks.
Can you fully recover from Parsonage-Turner syndrome?
Recovery from Parsonage-Turner syndrome can vary greatly. While some individuals may experience a complete recovery with no lasting effects, others may continue to struggle with weakness, pain, or disability. Early intervention with targeted rehabilitation exercises can significantly improve outcomes, but unfortunately, some may experience recurrent episodes or have lingering symptoms.
What triggers Parsonage-Turner syndrome?
The exact cause of Parsonage-Turner syndrome remains largely unknown. It’s believed to be triggered by an autoimmune response following factors such as viral or bacterial infections, surgery, vaccinations, childbirth, spinal taps, strenuous exercise, or other medical conditions. In many cases, however, no specific trigger is identified.
Can I exercise with brachial neuritis?
Yes, exercising with brachial neuritis is possible, but it should be done under the guidance of a healthcare professional. The focus should be on gentle movements to maintain range of motion and gradually strengthen the affected muscles without causing further pain or nerve damage.
What are the best exercises for a brachial plexus injury?
For a brachial plexus injury, effective exercises include:
- Range of motion exercises: Gentle stretching to keep the joints flexible.
- Strengthening exercises: Light resistance bands or weights to build muscle strength slowly.
- Neurological exercises: Techniques like tactile cues and proprioceptive training to improve nerve function and sensory-motor integration.
- Shoulder girdle exercises: Strengthening the muscles around the shoulder to support and stabilise the area.
What is the prognosis for Parsonage-Turner syndrome?
The prognosis for Parsonage-Turner syndrome varies widely. Many people see significant improvement within one to two years, but some may have persistent symptoms or recurrent episodes. Early diagnosis and proper treatment, including physical therapy, are crucial for better long-term outcomes.
Can Parsonage-Turner syndrome affect legs?
While Parsonage-Turner syndrome primarily impacts the brachial plexus in the shoulders and arms, it can sometimes affect other nerves, including those in the legs, although this is less common.
How do you recover from Parsonage-Turner syndrome?
Recovery involves a combination of rest, pain management, physical therapy, and sometimes medications like steroids to reduce inflammation. Rehabilitation focuses on restoring muscle strength, improving nerve function, and maintaining range of motion.
Can Parsonage-Turner syndrome be permanent?
In some cases, Parsonage-Turner syndrome can cause lasting damage, resulting in ongoing pain, weakness, or disability. However, many individuals achieve significant recovery with early intervention and proper management, allowing them to lead relatively normal lives.
Is Parsonage-Turner syndrome worse at night?
Pain from Parsonage-Turner syndrome can often be worse at night, likely due to decreased distractions and the body’s natural rhythms, which can make pain sensations more pronounced. Additionally, certain positions while lying down might exacerbate nerve compression, increasing discomfort.
How many people get Parsonage-Turner syndrome a year?
Parsonage-Turner syndrome is relatively rare, with an estimated incidence of 1-3 cases per 100,000 people annually. However, it may be underdiagnosed due to its rarity and variability of symptoms.
Does neuropathy get worse when lying down?
Neuropathy symptoms can worsen when lying down due to changes in blood flow, nerve compression, and the absence of distractions, making pain more noticeable. This can be particularly true for conditions like Parsonage-Turner syndrome, where nerve pain is a significant symptom.