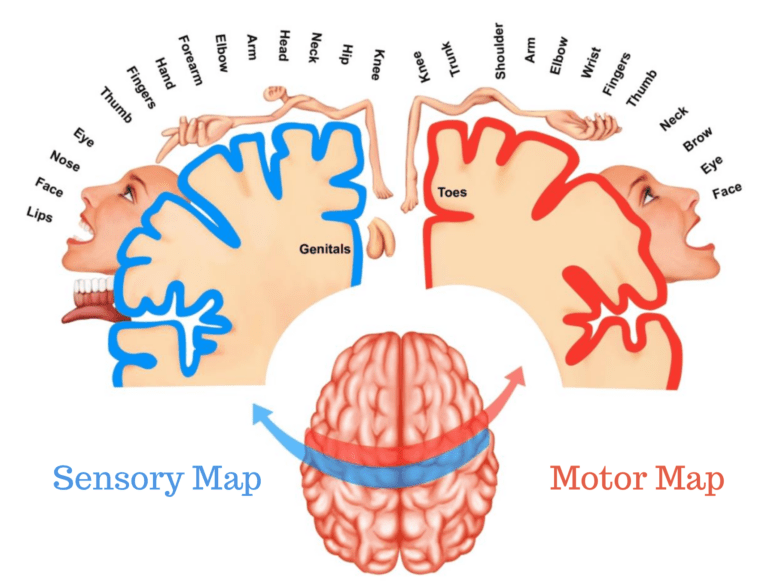
- Hypermobility and Exercise Part 2: Proprioception, Brain Maps and Why Your Body Feels Lost - 19 May 2026
- Hypermobility, EDS and Constipation: Why Your Gut Won’t Cooperate and What Actually Works - 18 May 2026
- Why Your Hypermobile Muscles Feel Tight and Weak at the Same Time: Understanding Muscle Tone - 14 May 2026
This article is part of our comprehensive guide to hypermobility and Ehlers-Danlos syndrome.
A well-balanced diet is essential to our health, but with conditions such as Ehlers-Danlos Syndrome (EDS) and Hypermobility Spectrum Disorder, the topic of diet can be fraught with pitfalls and disappointment. What works for one may not necessarily work for others, and with co-morbidities such as Mast Cell Activation Disorder, slow gut mobility, and a whole host of other issues, finding a hypermobility diet that agrees with you as an individual can be somewhat daunting.
The saying, “You are what you eat,” has a profound significance when navigating the challenges of conditions like EDS and hypermobility. Nutrition isn’t merely about sustenance; it’s a potent tool for symptom management, health improvement, and life enhancement.
Our previous exploration into the role of diet in managing EDS and hypermobility was a stepping stone, a starting point that sparked conversations and raised awareness. However, we realized that there was a need for more depth, nuance, and actionable insights. The EDS community deserved a comprehensive, research-backed, and practical guide to nutrition, and we were determined to deliver it.
At The Fibro Guy, we have qualifications in nutrition, but our scope mainly revolves around pain and joint stability. So, to provide the most value-driven information about hypermobility and diet, we contacted Katie Mednick, a registered dietitian specialising in hypermobility and EDS nutrition. Her expertise and our commitment to the EDS community have resulted in this revamped and enriched blog post centred around diet.
Our goal? To empower you with the knowledge you need to make informed dietary choices that can help manage EDS and hypermobility symptoms while helping you avoid various pitfalls, FADs, and downright harmful information, for the years ahead, for those aging with EDS.
This blog post is more than just a rewrite of the old one; it’s a testament to our dedication to serving the EDS community with the best resources and information, and we thought Katie was the best woman for the job to help.
So, whether you’re new to the EDS community, a long-time warrior, or a loved one seeking to understand and support in the areas of hypermobility/Ehlers-Danlos syndrome diets, this blog is for you. We’ll delve into the role of nutrition in EDS and hypermobility management, address common nutritional deficiencies, and provide practical diet recommendations and strategies.
This article covers:
Roadblocks to the Hypermobile diet
One of the key nutritional challenges for individuals with EDS and hypermobility is managing gastrointestinal symptoms like acid reflux and nausea, this can make the consumption of certain foods rather difficult. Often, individuals can struggle immensely with just maintaining adequate nutrition due to symptoms like poor appetite, nausea, fatigue, or even gastro pain.
It’s also not uncommon for individuals with EDS to self-impose restrictive diets in an attempt to help manage symptoms. While this approach may offer temporary relief, it can lead to nutritional deficiencies over time, potentially exacerbating symptoms like fatigue and weakness.
On top of everything already mentioned, we also have an abundance of misinformation about what diets or supplements are beneficial for EDS, ranging from things like creatine monohydrate, collagen, and floate, to untested protocols that claim to change the physical genetic makeup of sufferers! Very often this information is spread by social media, leading individuals down a path of unhelpful or even harmful dietary practices, all while making your bank account smaller and smaller.
As stated before, unfortunately, for those with Ehlers-Danlos syndrome or Hypermobility who do have issues around Diet, there are going to be a few roadblocks to their nutrition, things that can cause issues with EDS weight gain/loss, these issues can include:
- IBS: Current evidence would suggest that up to 62% (1). of patients with Hypermobile. EDS (HEDS) suffer from irritable bowel syndrome (IBS). However, despite the recognition of the presence of IBS in those with hypermobility, this overlapping group has not been especially characterized, meaning patients with Hypermobility and Ehlers-Danlos Syndrome have been managed in a similar way to those with IBS alone. One study found that nearly all subjects (98%) with hypermobility spectrum disorder met the criteria for Adult Functional Gastrointestinal Disorders, and when we take this into account, the idea of finding the best diet for hypermobility starts to look a lot more complicated (2).
- GI symptoms: Ehlers-Danlos Syndrome can significantly impact bowel and gastrointestinal function due to the laxity of connective tissue, making gut motility slower. Additionally, EDS types IV or vascular EDS have been shown to present a higher gastrointestinal bleeding and bowel perforation rate. Moreover, multiple studies show that GI symptoms are relatively common among patients with Hypermobility, with one study finding that 76.2% of the study group had some form of dysmotility, 42.8% had gastroparesis, 11.9% had short bowel/colon altered transit time, and 9.5% had global dysmotility (3). Likewise, a surprising finding from his study was that Postural Orthostatic Tachycardia (POTS) was also an independent predictive factor for GI dysmotility.
- Dyspepsia: Also known as indigestion, refers to discomfort or pain that occurs in the upper abdomen, often after eating or drinking. In one study of 62 functional dyspepsia patients, it was found that hypermobility was diagnosed in 55% of them (4). Dyspepsia, as a whole, is very unpleasant and can often contribute to certain negative behavioural changes around food, with many beginning to eat less and less to avoid symptoms.
- Postural Orthostatic Tachycardia (POTS): With POTS comes lightheadedness, palpitations, tremulousness during standing, and dizziness, all leading to a huge drop in appetite (understandably). However, this can cause more issues for those with hypermobility as their diet becomes affected. Water and salt help increase blood volume, which in turn helps lessen POTS symptoms. Additionally, low blood Co2 is also a huge issue with Pots, so I would recommend looking into this as well. However, with the symptoms already discussed, finding the appetite to sit down and eat can become a fairly arduous task.
- Mast Cell Activation Syndrome (MCAS): Mast cells have an important role in the body, including hosting defence to parasitic infection and in allergic reactions. As mast cells are key players in the inflammatory response, they can be activated to release various inflammatory mediators by many different antigens, including allergens, pathogens and physiological mediators. Some people with MCAS may have symptom improvement when they reduce their intake of foods with high histamine content. Since histamine is one of the mediators mast cells release, it can cause symptoms like rashes, hives, diarrhoea, etc. So, reducing histamine intake may be helpful for some people.
Living with EDS or Hypermobility Spectrum Disorder (HSD) often comes with a barrage of unsolicited advice, often including the idea of a specific EDS diet, However, it’s so important to dispel this myth, in order that we can avoid the potential hard that awaits this terrible advice!
There is no universally prescribed diet for EDS or HSD. In fact, there’s no medical justification for individuals with these conditions to categorically avoid certain foods based on their diagnosis alone. I really want you to read that again: there’s no medical justification for those with EDS to avoid certain foods.
Now then, let’s not take this advice the wrong way first off. What this means is that people should focus on nutrition on a person by person basis, and not because they have EDS or hypermobility. If you look at member of the general population, some can eat gluten, some cant. Some do much better with less carbs in their diet, and some do better with more. Nutrition, at the end of the day, is all about individuality.
Just because you have EDS doesn’t mean you need to follow a specific diet, your nutrition should be based upon what you need as an individual, and EDS may impact this area for you, but not in another individual. The decision to exclude specific foods from your diet should be a personal one, grounded in your experiences and guided by professional advice. If certain foods consistently trigger discomfort, it’s worth discussing this with a healthcare professional. Similarly, if you have a diagnosed food allergy, it’s essential to avoid allergenic foods to prevent adverse reactions.
Remember that certain health conditions can co-exist with EDS and HSD, such as irritable bowel syndrome (IBS), Gastroesophageal Reflux Disease (GERD), or Celiac Disease, and may necessitate specific dietary adjustments. In these instances, professional guidance can be a huge help to navigate your dietary choices without compromising on your nutritional needs.
When is a Specific Diet Necessary for EDS?
Nutritional deficiencies can cause a range of symptoms, but the most common one is fatigue. This is especially true for people with Ehlers-Danlos Syndrome (EDS) and Joint Hypermobility Syndrome, who often experience fatigue and may have difficulty absorbing essential vitamins and minerals.
Three of the most important nutrients that people with EDS and hypermobility need to be aware of are vitamin D, B12, and iron. Vitamin D is essential for bone health and a strong immune system, while vitamin B12 is necessary for cognitive function and for reducing symptoms of fatigue and depression. Iron is vital for carrying oxygen in the blood and maintaining immune function.
If you have EDS or hypermobility and experience fatigue, it’s worth checking for potential deficiencies and working with healthcare professionals to ensure you get the nutrients your body needs to function optimally.
It’s a question that’s been on many minds for a long time. While there’s no golden ticket or magic “EDS diet” waiting in the wings, there are an abundance of nutritional insights that can help to guide us when a specific diet may be something we should talk to someone about, these can include:
- Food Intolerances and Allergies:
Food intolerances and allergies are challenges that many face, regardless of their overall health status. For individuals with Ehlers-Danlos Syndrome or Hypermobility Spectrum Disorders, these dietary hurdles can add another layer to their daily management of symptoms.Lactose intolerance, for instance, is a common issue where the body struggles to digest lactose, a sugar found in milk and dairy products. Symptoms can range from bloating and gas to diarrhoea, often occurring a few hours after consuming lactose-containing foods or drinks. For someone with EDS, this can exacerbate the discomfort they might already be experiencing due to their condition.
On the more severe end of the spectrum, we have conditions like Celiac disease. This autoimmune disorder is triggered by ingesting gluten, a protein found in wheat, barley, and rye. When someone with Celiac consumes gluten, their immune system reacts by damaging the lining of the small intestine. This not only leads to gastrointestinal symptoms but can also result in long-term complications if not addressed. For an individual with EDS, managing Celiac becomes another crucial aspect of their health journey.
Another significant concern for the EDS community is Mast Cell Activation Disorder (MCAD). Mast cells play a vital role in our immune response, but in MCAD, they become overactive, releasing excessive amounts of histamine and other chemicals into the bloodstream. This can lead to many symptoms, from skin rashes and abdominal pain to fatigue and headaches. For those with EDS, who might already be managing a myriad of symptoms, MCAD can add another layer of complexity. One of the primary dietary interventions for managing MCAD, which many people find helpful (although not all) is adopting a low histamine diet. This involves avoiding foods high in histamines or triggering histamine release. Examples include aged cheeses, smoked meats, certain vegetables like eggplants, and alcoholic beverages.
It’s essential to understand that these food reactions and immune responses aren’t merely about discomfort, as over time, continually consuming foods that one is intolerant or allergic to or that trigger mast cell activation can lead to inflammation, nutrient deficiencies, and other health complications. For those with EDS or HSD, this can compound their daily challenges. Recognising and addressing these food intolerances, allergies, and immune responses is paramount. It often starts with keen observation, noting when symptoms flare up and what was consumed prior. Medical tests, such as blood tests for allergies or breath tests for lactose intolerance, can provide more definitive answers. Once identified, working with a nutritionist or dietitian can help craft a diet that avoids these triggers while ensuring all nutritional needs are met.
- Nutritional Deficiencies: Very often for those in the community, blood tests can reveal some large nutritional deficiencies which may necessitate the need for dietary changes. One of the most frequently observed deficiencies in the EDS community is iron. Iron plays a pivotal role in our body, aiding in the production of red blood cells and ensuring oxygen is efficiently transported throughout the body. A deficiency can lead to symptoms like fatigue, paleness, shortness of breath, and even hair loss. For someone with EDS, these symptoms can compound the challenges they already face daily.
Dietary changes can be a frontline approach. Incorporating iron-rich foods becomes paramount. This might mean adding more lean meats like beef or chicken liver to one’s diet. For vegetarians or those who prefer plant-based sources, foods like lentils, chickpeas, spinach, and fortified cereals can be beneficial. Combining these with vitamin C-rich foods, such as oranges or bell peppers, can enhance iron absorption, making the dietary changes even more effective.
However, introducing an iron supplement might be recommended in cases where the deficiency is pronounced or when dietary changes aren’t sufficient. It’s crucial to note that iron supplements should be taken under the guidance of a healthcare professional, as excessive iron can have adverse effects. It’s worth noting that iron isn’t the only nutrient of concern. EDS individuals might also face deficiencies in other vitamins and minerals, such as vitamin D or magnesium. Each deficiency presents its own set of challenges and requires a tailored approach to ensure the individual’s overall well-being.
- Chronic Conditions: For many individuals with Ehlers-Danlos Syndrome (EDS), the challenges don’t stop at joint hypermobility or skin elasticity. Many EDS patients also grapple with other chronic conditions, each bringing its own set of dietary considerations.
Take, for instance, diabetes. This condition, marked by the body’s inability to regulate blood sugar levels effectively, necessitates a careful approach to diet. An individual with both EDS and diabetes would need to be particularly mindful of their carbohydrate intake, ensuring they balance it with their insulin or other diabetes medications. They’d also need to monitor their blood sugar levels regularly and might benefit from consuming meals at consistent times. Foods rich in fiber, such as whole grains, legumes, and vegetables, would be encouraged, while sugary snacks and beverages might be limited.
High blood pressure, or hypertension, is another condition that can coexist with EDS. Dietary management for hypertension often revolves around the DASH (Dietary Approaches to Stop Hypertension) diet. This diet emphasises consuming fruits, vegetables, lean proteins, and whole grains while reducing sodium, saturated fats, and cholesterol. For someone with both EDS and hypertension, reducing their intake of processed foods, which are often high in salt and unhealthy fats, would be crucial. They might also be advised to incorporate potassium, magnesium, and calcium-rich foods, such as bananas, leafy greens, and dairy or fortified alternatives.
Again, some EDS patients might be diagnosed with Postural Orthostatic Tachycardia Syndrome (POTS), a condition where standing up from a lying position can cause a rapid increase in heart rate. One of the dietary recommendations for POTS is an increased sodium intake. This might seem counterintuitive, especially when the general advice leans towards reducing salt. However, for POTS patients, higher sodium can help increase blood volume, making it easier for the heart to pump blood. They might be advised to incorporate more broths, consume saltier snacks, or even add a bit more salt to their meals under medical supervision.
- Constipation: It’s a topic many shy away from, but for many individuals with Ehlers-Danlos Syndrome, the shadow of chronic constipation looms large. As constipation can be a common ailment in the community, it may be a factor that necessitates following a specific diet to address it.
So, what’s the connection between a collagen disorder like EDS and a digestive issue like constipation? The answer might lie in the intricate dance between our gut and brain, the gut-brain axis. This axis represents the communication network that exists between our digestive system and our central nervous system. For those with EDS, emerging evidence suggests that a dysfunction in this network could be at play. Such dysfunction can lead to altered nerve signals responsible for the rhythmic muscle contractions in the gastrointestinal tract. And also cause an increase in sensory processing of pain. When these contractions are out of sync, slower, or weaker, food moves at a reduced pace through the digestive system, culminating in constipation.
But the challenges don’t stop at irregular bowel movements. The repercussions of constipation extend to lower gastrointestinal discomfort, a bloated sensation, and the often strenuous effort required during bowel movements. Moreover, this constipation can be intricately linked with gas pains, adding another layer of discomfort to the mix.
Diet and lifestyle play pivotal roles in managing this symptom. A diet that skimps on fibre or doesn’t prioritise hydration can exacerbate constipation. On the flip side, being sedentary can compound the issue, as regular movement aids the natural progression of food through the digestive tract. Addressing constipation, especially in EDS, requires a multifaceted approach. Dietary adjustments can be beneficial, such as increasing fibre intake and ensuring adequate fluid consumption. Incorporating gentle, regular, hypermobile exercises can also promote better digestion. For some good tips for exercise check out our hypermobile exercise tips article, covering cortical mapping. And in some instances, medical interventions, be it over-the-counter remedies or prescribed medications, might be the way forward.
Hydration, PoTs and Sodium Intake
No article about hypermobility and diet would be complete without at least touching on hydration. But, for those with Ehlers-Danlos Syndrome and Hypermobility, this is an especially important topic!
Postural Orthostatic Tachycardia Syndrome, commonly known and referred to as POTS, is a condition that is intricately linked with Ehlers-Danlos Syndrome. At its core, POTS is characterised by a significant increase in heart rate when a person transitions from sitting to standing. This sharp rise in heart rate is often accompanied by symptoms such as dizziness and/or even fainting. However, what does this have to do with hydration and sodium, and why are these elements crucial for those with EDS and hypermobility?
Well, it starts with electrolytes, which are minerals like sodium, chloride, potassium, calcium, and magnesium. These electrolytes play a pivotal role in our body as they are responsible for a few fairly important tasks such as transmitting nerve impulses, contracting muscles, and most importantly for our discussion, maintaining fluid balance. Sodium, in particular, is a standout player when it comes to fluid balance. It aids the body in retaining water. This relationship between sodium and water is quite symbiotic: as sodium intake increases, the amount of water retained by the body also rises. This water retention subsequently boosts the overall blood volume, which is precisely what individuals with POTS desire to alleviate their symptoms.
Research has indicated that many POTS patients grapple with maintaining fluid balance, and this imbalance, often manifests as hypovolemia, a condition characterized by low blood volume. There are of course, several factors that can lead to hypovolemia for those with POTS, including, but not limited to, impaired function of the renin-angiotensin-aldosterone system, excessive fluid loss due to diarrhoea, or insufficient fluid and electrolyte intake caused by chronic nausea.
So then, how do electrolytes, and particularly sodium, assist those with POTS in combating hypovolemia? The answer lies in the body’s natural response to electrolyte consumption, as when we consume electrolytes, our body retains the water we drink, leading to an increase in blood volume. This means that a combination of electrolytes and proper hydration can significantly improve hypovolemia.
The Role of Sodium in POTS Management
Many institutions aimed at managing POTS recommend that individuals with POTS should aim for a sodium intake of about 3,000-10,000 milligrams per day. This recommendation stems from the understanding that sodium helps the body retain water, increasing blood volume. It’s essential to differentiate between salt and sodium. Salt is composed of 50% sodium and 50% chloride. Therefore, when considering sodium intake, it’s crucial to account for this distinction.
Likewise, for those with POTS, striving to consume about 2-2.5 litres (approximately 8.5-10.5 cups) of fluids daily seems to be the general consensus. This fluid intake can come from various sources, including sports drinks, juices, teas, broths, and water. Proper hydration, combined with the right sodium intake, can significantly alleviate the symptoms of POTS.
A study conducted in 2003 on 22 healthy individuals (without POTS) revealed the profound impact of water on the body’s ability to stand for extended periods (5). Participants who drank water before undergoing a tilt table test (a diagnostic test for POTS) were able to tolerate the test 36% longer than those who didn’t. This study underscores the importance of hydration in regulating heart rate and maintaining effective circulatory function.
The intricate relationship between EDS, hypermobility, and POTS makes managing fluid and sodium balance even more crucial. Proper hydration and sodium intake not only help manage POTS symptoms but also play a vital role in ensuring the overall well-being of those with EDS and hypermobility.
Potentially go gluten-free for POTS
In light of a new area of research, a new study looking at the impact of a gluten-free diet (GFD) on POTS patients offers promising insights, revealing that following a GFD for just four weeks, a significant reduction in POTS symptoms occurred, particularly in areas such as dizziness, blood flow issues, and gastrointestinal discomfort (6). This suggests that dietary adjustments, like eliminating gluten, may play a role in alleviating some of the burdens associated with POTS. However, it is important to remember that this study was a very small sample size, and further studies are needed to confirm these findings over the long term. However, initial results are encouraging.
Things to Consider as part of your Hypermobility Diet
As you can see from the paragraphs above, we are left with a big hole in our dietary plan when we consider other comorbidities. Given the issues we have covered, and depending on you and your symptoms, what can we consider helping with our hypermobility diet?
- Water: As mentioned earlier, increasing your intake of water can help with conditions associated with Hypermobility and Ehlers-Danlos such as POTS. When water loss exceeds intake, blood volume decreases and plasma osmolality increases causing problems for those with hypermobility. By increasing your water intake you can dramatically increase your standing blood volume. It’s also pertinent to remember that every chemical reaction within the body requires water to happen, and only a slight drop in water can dehydrate our GI tract resulting in the large intestine (colon) soaking up whatever water it can from the food you consume, making it too hard to pass, causing pain and constipation (7). Foods such as soups have also been proven to help with POTs, which can make the hypermobile diet a little easier by allowing us to eat something that can be digested easier.
- Sodium: Simply put, the more sodium in your body, the means more circulating volume you have, which means a better tolerance level for being upright when we take into account issues such as POTS. An increase of salt will also cause vasoconstriction, helping to reduce the amount of venous pooling (extra blood that collects in the veins) in the legs, whilst also increasing your blood volume and preventing a drop in your blood pressure. The recommended sodium intake for the non-hypermobile population in the UK is 6 grams, however, for those with hypermobility and EDS, 6-8 seems to be recommended, even pushing up to 5-10g/day for very symptomatic patients. However, in America, it is recommended at about 2,300mg/2.3g of sodium for healthy adults, and 3-10g of sodium for POTS patients (8).
- Avoid alcohol: Alcohol frees histamine from its mast cell stores and depresses histamine elimination by inhibiting diamine oxidase, resulting in elevated histamine levels in tissues. When we combine this with issues such as Mast cell activation disorder, it is truly a recipe for disaster. Alcohol can also prevent blood vessels from vasoconstriction as normal, diminishing the return of the blood to the heart and brain which may lead to worsening of POTS symptoms. Likewise, alcohol is a diuretic, which can lead to dehydration, worsening some of the issues mentioned above. It is also worth noting that some research that exists finds a link that suggests that women with hypermobility tend to use alcohol more frequently than their non-hypermobile counterparts.
- Protein: Proteins are essential dietary components that are pivotal in various bodily functions. Composed of chains of amino acids, proteins are the building blocks for tissues, enzymes, hormones, and other crucial molecules. While the body can produce some amino acids, others, termed essential amino acids, must be sourced from our diet. These amino acids are vital for the body to produce the proteins required for countless functions, including collagen synthesis, which is particularly relevant for individuals with EDS. Protein plays an even more significant role in the lives of individuals with EDS and hypermobility. These individuals often engage in rehabilitation exercises to enhance joint stability and reduce the risk of dislocations and pain. Consuming adequate protein ensures that the muscles have the necessary building blocks to recover and strengthen, aiding overall rehabilitation.
While there’s no specific protein requirement unique to EDS patients, it’s essential to understand that a professional might need to tweak your protein needs based on your activity level, type of exercise, illnesses like infections, healing from injury, etc.
The Gap in Research for EDS and Diets
The realm of medical research is vast, with numerous studies delving into various health conditions and their treatments. However, when it comes to diets tailored for hypermobility and related conditions like Ehlers-Danlos Syndrome, there’s a noticeable gap in comprehensive research, which unfortunately, does not seem to be getting smaller anytime soon.
While there are many studies on general nutrition and its impact on a range of health conditions, specific research focusing on hypermobility diets remains limited. One of the challenges in this area is the heterogeneity of symptoms among individuals with hypermobility. This makes it difficult to standardise a diet for research purposes.
We then have the fact that hypermobility and EDS are complex multifaceted conditions, influenced by various genetic, environmental, and lifestyle factors. Isolating the impact of diet alone can be a fairly complex endeavour!
Yet, the lack of robust research means that individuals with hypermobility often rely on anecdotal evidence or general dietary advice, and while general nutrition guidelines can be beneficial, they probably won’t address the unique challenges faced by those with hypermobility or EDS. As we will discuss later, this gap in research can also lead to misinformation, with patients potentially adopting diets that might not be beneficial or, in some cases, could be harmful. There’s a clear need for more rigorous, large-scale studies focusing on hypermobility diets. Such research can provide evidence-based guidelines for individuals with hypermobility, ensuring they receive the best possible dietary advice tailored to their needs.
One area, however, that has had some research into is the area of FODMAP’s, so let’s take a peek at what it says!
So what is the FODMAP diet?
FODMAP is not a single entity, but a group of compounds, including oligosaccharides (fructans, fructo-oligosaccharides = FOS and galacto-oligosaccharides = GOS), disaccharides (lactose), monosaccharides (fructose), and polyols (sorbitol, mannitol, maltitol, xylitol, polydextrose, and isomalt).
This rather long-winded acronym refers to foods classed as short-chain carbohydrates, or in other words, sugars that aren’t very well absorbed in the small intestine, meaning they force water into your digestive tract, and your gut bacteria ferments them, increasing gas and short-chain fatty acid production (9). People are generally assigned to a FODMAP diet to eliminate these foods as a means of reducing symptoms of irritable bowel syndrome (IBS) and small intestinal bacterial overgrowth (SIBO).
This diet, in particular, seems to be well received by those with those in the community who suffer from GI symptoms. However, it’s always important to note, that working with a professional when it comes to your diet is going to be far more efficient and safer than going it alone. Nutrition is individual, and for every person that swears by the FODMAP diet, there will be another who does not.
Research suggests that a strict long-term, low-FODMAP diet may negatively impact the intestinal microbiome. After the initial strict period (which we will talk about in a moment) the FODMAP diet should be followed up by relaxed FODMAP restriction that enables the inclusion of prebiotic FODMAPs while still maintaining symptom relief.
With many anecdotal reports, and indeed some very interesting research, the FODMAP diet seems to be helping a lot of people with hypermobility and EDS. We could perhaps even say that it is quickly becoming considered a first-line dietetic intervention for people with EDS.
Whilst not an amazing body of research exists for the FODMAP diet, many studies have demonstrated that the low FODMAP diet achieves a significant improvement in symptoms such as bloating, IBS, abdominal pain, and flatulence, in those with hypermobility compared to a standard diet (11).
Studies also suggest that a low FODMAP diet has greater improvement in hypermobility patients than non-hypermobile patients when it comes to issues such as IBS symptoms (pain, diarrhoea, bloating and constipation) (12).
This, of course, comes as no great surprise, considering how many of those with hypermobility have gastrointestinal symptoms, so anything focused on helping these areas is bound to be received well. What we here at The Fibro Guy like about the FODMAP diet, is that it is especially low in histamine, and has the potential to reduce debilitating symptoms of conditions like MCAS.
How do you do the low FODMAP diet?
As far as hypermobility diets go, the low FODMAP diet is pretty easy to follow. What people seem to struggle with is the sheer restrictions on this diet, which is understandable as there are a lot!
However, if you can muster the willpower to get through this diet, the evidence shows that for some, it may promise to be effective at reducing symptoms.
The FODMAP diet is a three-phase approach designed to help individuals identify and manage foods that trigger gastrointestinal symptoms. Here’s a detailed guide on how to follow the FODMAP diet:
Phase 1: Elimination
In this initial phase, all high FODMAP foods are eliminated from the diet for a period of 2-6 weeks. This allows the gut to calm down and symptoms to settle. It’s important to note that this is not a long-term solution, but a temporary measure to reset the gut.
High FODMAP foods to avoid during this phase include:
- Certain vegetables like garlic, onions, artichokes, asparagus, baked beans, beetroot, black-eyed peas, broad beans, butter beans, cauliflower, celery (greater than 5cm of stalk), and many more.
- Fruits such as apples, apricots, avocados, ripe bananas, blackberries, cherries, custard apples, dates, figs, grapefruit (over 80g), and others.
- Dairy products high in lactose like buttermilk, ricotta cheese, cream, custard, gelato, ice cream, and certain types of milk (cow, goat, sheep’s, evaporated).
- Protein sources like chorizo (if garlic added), sausages, and certain legumes/pulses.
- Breads & cereals made from wheat/rye/barley, certain breakfast cereals, biscuits, and snack products.
- Sugars, sweeteners, and sweets that contain high fructose corn syrup (HFCS), honey, inulin, isomalt, lactitol, maltitol, mannitol, sorbitol, xylitol, and others.
- Certain types of drinks and protein powders like beer (if drinking more than one bottle), certain fruit juices, kombucha, meal replacement drinks containing milk-based products, rum, sodas containing HFCS, certain types of tea, and whey protein (unless lactose-free).
One thing which can be frustrating is that many sources differ in what they do and do not class as low FODMAP. For a comprehensive list of high FODMAP foods, you can refer to this FODMAP Food List (13).
Phase 2: Reintroduction
After the elimination phase, you will start to reintroduce foods back into your diet one at a time. This phase can take anywhere from 6 weeks to 3 months. The goal is to identify which foods trigger symptoms. This is usually done with the help of a dietitian.
Phase 3: Personalization
Once you’ve identified which foods trigger symptoms, you can start to personalize your diet. This means avoiding or limiting your intake of the foods that cause symptoms, while freely eating the foods that don’t. The goal is to have a varied, enjoyable diet that keeps your symptoms under control.
Remember, everyone’s tolerance to different foods will vary. It’s important to listen to your body and adjust your diet accordingly. It’s also recommended to seek guidance from a healthcare professional or dietitian when following the FODMAP diet to ensure you’re getting all the necessary nutrients.
Nutritional Deficiencies in EDS
Nutritional deficiencies can manifest in various ways, but one of the most pervasive symptoms is fatigue. This is particularly relevant for individuals with Ehlers-Danlos Syndrome and Joint Hypermobility Syndrome, who frequently grapple with fatigue and may encounter challenges in absorbing essential vitamins and minerals. Three critical nutrients that individuals with EDS and hypermobility should monitor are vitamin D, vitamin B12, and iron.
Vitamin D: The Sunshine Vitamin
Vitamin D, often dubbed the “sunshine vitamin,” is a fat-soluble vitamin predominantly produced by our bodies when exposed to sunlight. It can also be found in a limited number of foods, such as fatty fish, egg yolks, and fortified dairy products.
There are two primary forms of vitamin D: D2 (ergocalciferol) and D3 (cholecalciferol). Vitamin D3 is the form our skin synthesizes when exposed to sunlight, while D2 is primarily found in plant-based sources.
Vitamin D plays a crucial role in calcium absorption and bone mineralization, helping to maintain the strength of our bones and teeth. It also supports healthy muscle function and a robust immune system, which is particularly important for individuals with EDS/hypermobility.
Katie also suggests that from her experience, it seems like patients who don’t feel well don’t eat well. By choosing comforting/convenient/processed foods most of the time, it’s hard to get enough vitamin D.
Vitamin B12: Essential for Cognitive Function
Vitamin B12 is an essential nutrient that plays a crucial role in many bodily processes. It is necessary for the production of red blood cells, DNA, and the proper functioning of the nervous system. However, many with hypermobility/EDS report deficiency in vitamin B12. Of note, a deficiency here can lead to a condition called megaloblastic anaemia, which is characterised by fatigue, weakness, and shortness of breath.
It may be important to note here, that many of those with EDS are also diagnosed with Fibromyalgia, and a very recent study aimed to investigate the correlation between vitamin B12 deficiency and fatigue, as well as other neurologic symptoms in patients with fibromyalgia (14). The study included a retrospective analysis of the medical records of 2142 fibromyalgia patients who were diagnosed between 2015 and 2020. The results of the analysis showed that 42.4% of the patients had a B12 deficiency, and that fatigue and memory loss were more common in the B12 deficiency group. After adjusting for vitamin D levels, B12 deficiency remained significantly associated with the presence of fatigue. This study provides the first evidence for an association between B12 deficiency and fatigue in fibromyalgia patients.
B12 is a vital nutrient for maintaining good cognitive function, reducing depressive symptoms, and preventing fatigue. However, for those with hypermobility, these symptoms are often experienced even in the absence of vitamin B12 deficiency or neurological disorders. The effectiveness of vitamin B12 supplementation in such cases has been a subject of debate.
Another recent study aimed to assess the effects of vitamin B12 alone or in combination with folic acid and vitamin B6 on cognitive function, depressive symptoms, and idiopathic fatigue in patients without advanced neurological disorders or overt vitamin B12 deficiency (15).
The study was a systematic review and meta-analysis of randomized controlled trials (RCTs) that were searched through various databases, including Medline, Embase, PsycInfo, Cochrane Library, and Scopus. The researchers included 16 RCTs with 6276 participants in their analysis. They found no evidence to support the effectiveness of vitamin B12 alone or in combination with folic acid and vitamin B6 on any subdomain of cognitive function outcomes.
Additionally, there was no significant association of treatment effects with any of the potential predictors and the study found no overall effect of vitamin supplementation on measures of depression. Unfortunately, only one study reported effects on idiopathic fatigue, so no analysis was possible.
Based on these findings, vitamin B12 supplementation alone is likely to be ineffective in improving cognitive function and depressive symptoms in patients without advanced neurological disorders. However, it’s important to note that vitamin B12 is still a necessary nutrient for overall health, and those with hypermobility should still aim to meet their daily recommended intake through their diet or supplements.
Keep in mind also, that It’s possible that people with hypermobility may develop B12 deficiencies from commonly used medications that interfere with the absorption of vitamin B12, like proton pump inhibitors or metformin
Iron: Vital for Oxygen Transport
Iron is an essential mineral that plays a critical role within our body, including carrying oxygen in the blood and helping to support immune function. However, iron deficiency is a common health problem worldwide, especially among women and children, and increasingly, those with hypermobility and Ehlers-Danlos syndrome.
Iron deficiency is a common cause of anaemia, a condition in which the body doesn’t have enough red blood cells to carry oxygen to the body’s tissues. When the body lacks iron, it is unable to produce enough haemoglobin, a protein in red blood cells that carries oxygen to the body’s organs and tissues. As a result, the body’s organs and tissues don’t get the oxygen they need, leading to fatigue, weakness, and other symptoms such as shortness of breath, dizziness, headache, pale skin, and rapid heartbeat. If left untreated, iron-deficiency anaemia can become severe and lead to complications such as heart problems, developmental delays in children, and even increased risk of infections.
Identifying and addressing nutrient deficiencies can significantly improve symptoms of fatigue for those with EDS and Joint hypermobility Syndromes. It is crucial to prioritize a nutrient-rich diet and work with healthcare professionals to ensure you are getting the nutrients your body needs to function optimally.
Protein Intake For Those With EDS/Hypermobility
Protein isn’t typically the nutrient that springs to mind when discussing nutritional deficits in Ehlers-Danlos Syndrome (EDS). Nevertheless, it is essential for general well-being, and not getting enough protein can worsen numerous symptoms commonly associated with EDS, such as lethargy, delayed healing, and weak muscles.
Interestingly, there’s no current scientific evidence suggesting that individuals with EDS require more protein than the general population. However, in clinical practice, many people with EDS seem to feel significantly better when they increase their protein intake. This isn’t because their protein needs are inherently higher; it’s because many aren’t meeting their baseline requirements in the first place.
This shortfall can happen for several reasons. Poor appetite, a frequent challenge in EDS, often means meals are skipped or portion sizes are smaller than they should be. Digestive discomfort, food sensitivities, or conditions like gastroparesis may lead individuals to avoid protein-rich foods like meats or legumes. Additionally, chronic fatigue and joint pain can make meal preparation exhausting, leading to reliance on convenience foods that are often low in protein.
The result is a subtle but persistent deficiency that can impact everything from energy levels to tissue repair.
Why Protein Matters in EDS
Amino acids are building blocks of proteins; however, there are some amino acids that the body needs from food because it cannot produce them internally. You can’t do without these amino acids because:
Repairing damaged tissues: facilitating the recovery of strained muscles, ligaments, and tendons.
While there is no evidence that taking collagen supplements will alleviate EDS, making sure you get enough protein in your diet will give your body what it needs to produce enough collagen.
Protein helps keep muscle mass, which is important for the stability of joints and general mobility; it also contributes to energy.
Protein cannot be stored for later use by the body like lipids and carbs can. Therefore, it is crucial to consume it regularly in order to avoid deficiencies.
Are You Eating Enough Protein?
To put it in perspective, protein requirements are usually determined by weight. Protein needs range from 0.8 to 1.2 grammes per kilogramme of body weight per day for adults, with the exact amount depending on things like activity level, healing from injuries, and recent illness.
For example:
- This requirement increases during recovery from injury, after surgery, or when experiencing illness or infection.
- A person weighing 150 pounds (68 kilograms) would require between 55–82 grams of protein daily to meet their needs.
Protein deficiency makes it difficult for the body to perform even basic maintenance tasks, let alone efficient tissue repair. Protein, whether consumed in the form of food, protein shakes, or supplements, improves energy levels, decreases muscle fatigue, and general well-being, which may explain why many people with EDS experience these benefits after increasing their protein intake.
Even though people with EDS don’t necessarily require more protein than the average person, many of them aren’t getting enough. Effects on vitality, tissue healing, and resistance to stress can be far-reaching due to this subtle deficit.
You may want to reconsider your protein consumption if you’ve been experiencing chronic tiredness, sluggish healing, or weak muscles. Meeting your daily needs for protein, whether that’s through eating more foods rich in protein, drinking protein shakes, or taking supplements, may have a significant impact on your day-to-day mood.
Supplements for EDS and Hypermobility
So, first off, we need to set the record straight, as this is definitely one of Katie’s biggest bugs. Supplements are supposed to be the cherry on top of your nutrition, complementing the diet, it’s all in the name really: supplement.
However, navigating the world of supplements can feel like a walk in the park on a sunny day or a trek through a dense, foggy forest, depending on how you approach it. There are a myriad of options available to people, and it leaves us dizzy with the questions of how does one discern which supplements are actually beneficial, especially for conditions like EDS and hypermobility?
So, let’s take a look at some of the most commonly talked about.
The Magnesium and EDS Relationship
Magnesium plays a crucial role in our body. For those with EDS, its importance is even more evident. A deficiency in magnesium can exacerbate some EDS symptoms. If you’re deficient, magnesium supplements might be beneficial.
Many EDS patients report constipation. Some magnesium supplements can help by retaining water in the intestines, making stools softer. However, it’s essential to find the right balance to avoid frequent bathroom trips.
Hydration is vital, especially for those with conditions like Postural Orthostatic Tachycardia Syndrome (POTS). Magnesium is included in electrolyte supplements to help replete magnesium lost in sweat. Some EDS patients also report migraines and headaches, which might be linked to magnesium deficiency. Certain magnesium supplements could help reduce these headaches. When considering magnesium supplements, it’s essential to find the right one for your needs. For example, Magnesium L-threonate and Magnesium glycinate might be beneficial for mood, while Magnesium oxide could help with constipation.
Collagen’s Role
Collagen is a vital protein in our body, providing structure and support. But for those with EDS, taking collagen supplements might not be the straightforward solution it seems. Our bodies break down ingested collagen, and genetic factors determine how it’s rebuilt. If there’s a genetic issue, as in EDS, the newly formed collagen might not function optimally. This means you are effectively throwing your money away on this supplement, and to date no data exists to show it works how many claim, this is down to the fact that a supplement cannot alter your genetics.
Vitamin C and Hypermobility
Historically, a lack of vitamin C led to conditions like scurvy among sailors. This vitamin is essential for collagen synthesis. There’s ongoing discussion in the medical community about the potential benefits of vitamin C supplements for those with EDS, but more research is definitely needed to back up the many claims around this supplement.
Psyllium Husk Fibre
Derived from the Plantago ovata plant, psyllium husk fibre can be beneficial for digestive health. It acts as a gentle regulator for the digestive system. Worth knowing though: in those with hypermobility, constipation often involves rectal hyposensitivity or dyssynergic defecation rather than simple slow transit, and in those cases adding fibre can make bloating worse rather than better. We’ve covered the mechanisms and the evidence in detail in our guide to constipation in hypermobility and EDS.
Vitamin D Insights
Vitamin D is known for its role in bone health and mood regulation. For the EDS community, it’s an area of interest, seeing as low bone mineral density and fractures seem to be frequent in some of the rare EDS types (kyphoscoliotic, arthrochalasia, spondylodysplastic, and classic-like EDS) (16).
Dangers of FAD diets, and unproven treatments
Now, there is one thing which can be even more dangerous than misuse and misinformation around supplements, and that FAD diets and unproven protocols. It is totally understandable for people to want to try as many things as they can that may help, even if it’s just based of anecdotal evidence, however, much caution is needed.
The Cusack Protocol is an example of an unproven protocol that has gained attention in some circles, especially on social media. Here are the potential dangers of relying on unproven protocols:
- Lack of Scientific Evidence: Unproven protocols often lack rigorous scientific evidence to support their claims. Without peer-reviewed studies and controlled trials, it’s difficult to determine the efficacy and safety of such protocols.
- Potential for Harm: Without proper testing and validation, there’s a risk that the protocol could cause harm or exacerbate existing conditions. This is especially concerning for individuals with underlying health conditions.
- False Hope: Relying on unproven protocols can give individuals false hope. When the desired outcomes are not achieved, it can lead to disappointment, frustration, and a sense of hopelessness.
- Wasted Resources: Investing time, energy, and money into unproven treatments can divert resources away from evidence-based treatments that might be more beneficial.
- Interactions with Other Treatments: Unproven protocols might interfere with or counteract other treatments a person receives, potentially diminishing their effectiveness or causing adverse reactions.
Dangers of Fad Diets
In our modern, fast-paced world, where instant gratification is often the order of the day, the appeal of fad diets is hard to resist. These diets, which often parade themselves as the ultimate solution to our weight and health challenges, have seen a surge in popularity. But, if we scratch beneath the surface, we’ll find that these seemingly magical solutions come with a host of hidden dangers:
Nutritional Imbalances
One of the most glaring issues with fad diets is the risk of nutritional deficiencies. When you start cutting out or severely limiting certain food groups, you’re not just missing out on some of your favourite dishes. You’re potentially depriving your body of essential nutrients it needs to function optimally. For instance, diets that advocate for minimal carbohydrates might seem like a quick fix, but in the long run, they can rob your body of vital nutrients found in fruits, vegetables, and grains. This deprivation can lead to deficiencies in essential vitamins, minerals, and dietary fibre, which in turn can have a cascade of negative effects on your health.
The Illusion of Short-Term Gains
Sure, fad diets can offer a tantalisingly quick drop in weight. But here’s the thing: they rarely, if ever, provide a lasting solution. Their focus is predominantly on immediate, often drastic results, sidelining the importance of cultivating long-term healthy eating habits. This narrow vision can lead individuals down the path of yo-yo dieting, a frustrating cycle of losing and regaining weight. This not only wreaks havoc on the body’s metabolism but can also be incredibly disheartening for the individual.
Potential Health Hazards
Beyond the risk of missing out on your favourite foods, extreme dietary restrictions can pose serious health threats. From the discomfort of dehydration to the more severe risks of malnutrition, the dangers are real and varied. And in some extreme cases, especially with diets that drastically cut down on carbohydrates, the body can enter a state of ketoacidosis. This isn’t just a fancy term; it’s a potentially life-threatening condition.
The Mental and Emotional Toll
The psychological implications of fad diets are profound, yet they often fly under the radar. By promoting an unhealthy relationship with food, these diets can lead to obsessions, guilt, and heightened anxiety around eating habits. Over time, this can snowball into more severe eating disorders, not to mention a distorted and unhealthy body image.
Promises, Promises
Fad diets are notorious for their grandiose promises. “Lose 10 pounds in a week!” or “Detox your body in just three days!” Such claims can be incredibly enticing. However, these unrealistic expectations can set individuals up for inevitable disappointment. When the results don’t match the hype, feelings of inadequacy and failure often follow.
The Financial Strain
Let’s not forget the economic implications. Many fad diets heavily promote expensive supplements, rare superfoods, or unique meal plans. While investing in health is commendable, pouring money into these often unproven and short-lived diets might not offer any substantial long-term benefits. It’s like buying a shiny new toy that loses its appeal in a few days.
While the allure of quick fixes is undeniable, it’s always worth remembering that good things take time. Instead of seeking shortcuts, it’s beneficial to invest time in understanding one’s body, seeking advice from trusted healthcare professionals, and adopting a balanced approach to health that’s sustainable in the long run.
Lifestyle Factors and EDS Management
Living with EDS and hypermobility is a unique experience, requiring a deep understanding and adaptation to one’s own body. The choices we make daily can have a profound impact on the symptoms associated with these conditions. Let’s delve deeper into these lifestyle factors.
Managing EDS symptoms isn’t just about medication or therapy; it’s about building a strong foundation of healthy habits:
- Prioritising EDS AND Sleep: Sleep is more than just rest; it’s a time for the body to heal and rejuvenate. For those with EDS, ensuring consistent and quality sleep is paramount. This means creating a sleep environment free from distractions, maintaining regular sleep schedules, and ensuring the body gets the recommended 7-9 hours of sleep. Over time, this can lead to improved energy levels, better cognitive function, and reduced pain sensitivity.
- Balanced Nutrition: A well-balanced diet is crucial for everyone, but for those with EDS, it can make a significant difference. This involves reducing processed foods and focusing on a mix of proteins, carbohydrates, fresh vegetables, and healthy fats. Additionally, understanding any food sensitivities and adjusting one’s diet can lead to better digestive health and overall symptom management.
- Alcohol Intolerance and Food Sensitivities
For many with EDS or hypermobility disorders, certain substances like alcohol or specific foods can trigger adverse reactions. These aren’t just minor discomforts; they can significantly disrupt daily life. It’s essential to identify these triggers. Some may experience heightened symptoms after consuming even small amounts of alcohol, while others might find that certain foods lead to digestive issues or heightened fatigue. By understanding and avoiding these triggers, we can better manage our symptoms.
- Staying Hydrated: Hydration plays a pivotal role in overall health. For those with EDS, it can help manage symptoms like fatigue and low blood pressure. This doesn’t just mean drinking when thirsty but ensuring consistent hydration throughout the day. This can involve drinking water, herbal teas, and other low-sugar beverages, and also being mindful of foods with high water content.
- Embracing Regular Physical Activity: Physical activity is beneficial for everyone, but for those with EDS, it can be transformative. Tailored Ehlers Danlos syndrome exercises, like low-impact activities such as swimming or cycling, can improve cardiovascular health, aid digestion, and strengthen muscles, which in turn can support vulnerable joints. Moreover, regular movement can help regulate blood sugar levels, supporting metabolic health.
Who should I see for my Diet?
Navigating the complex world of nutritional concerns requires a collaborative effort between dietitians and doctors when it comes to hypermobility and EDS. Their roles, though, whilst very distinct, intertwine seamlessly to ensure that individuals in the community receive comprehensive care, that is tailored to their individual circumstances.
Dietitians, play an important role in managing the myriad of gastrointestinal and other symptoms that very often accompany EDS. They can delve deep into the intricacies of an individual’s dietary habits, helping you to identifying potential triggers and deficiencies, and come up with a solid plan to address them. Their expertise doesn’t just stop at suggesting dietary modifications, as they can also assist in pinpointing the specific nutrition needs of an individual, ensuring that the body receives the right fuel to function optimally.
But it’s not just about what you eat; it’s also about how you eat. Recognising the challenges faced by many with EDS, dietitians often provide ingenious strategies to make nutrition accessible. Think of meal ideas that are not only nutritious but also require minimal physical effort, reducing the strain on hypermobile joints.
On the other side of the spectrum, we have doctors, they are the ones who delve into the nitty-gritty of medical testing, be it for nutritional deficiencies or gastrointestinal conditions like Small Intestinal Bacterial Overgrowth (SIBO), inflammatory bowel disease, and even ulcers. Their role doesn’t just end with diagnosis though. They also prescribe medications, ensuring that individuals receive the right treatment to manage their symptoms effectively.
Both dietitians and doctors play crucial roles, and when it comes to managing EDS and hypermobility-related nutrition concerns, it is most definitely a collaborative effort. It’s a dance between the expertise of these professionals and the lived experiences of individuals. Together, they create a symphony of care, ensuring that those with EDS not only survive but thrive.
In wrapping up our mammoth article on nutrition and its relationship with Ehlers-Danlos Syndrome and hypermobility syndromes, it’s paramount to understand that there isn’t a universal “best diet” for hypermobility. Each individual’s nutritional needs and responses can vary widely.
Those with EDS should approach their dietary choices with the same care and consideration as anyone else, focusing on a balanced and nutritious diet that caters to their unique requirements. It’s crucial to steer clear of fad diets or unverified claims, instead grounding one’s choices in sound nutritional science, using professionals to help you along the way.
Engaging with healthcare professionals, such as dietitians and doctors, can provide invaluable guidance in this journey. Ultimately, the aim isn’t to chase after a mythical perfect diet but to make informed and sustainable choices that bolster overall health and help manage the symptoms associated with EDS.
That’s all from us here at The Fibro Guy, we hope you enjoyed reading the new and improved diet article. A big shoutout to Katie for helping us ensure this article was sound and contained solid science-backed advice.
Until next time friends.
The Fibro Guy
Hypermobility Live Workshop
Do you find value in this content and the way we break hypermobility down into something you can actually understand and use? If so, imagine what you could get from spending four weeks inside our Hypermobility Live Workshop, where we go deeper into the frameworks, coach you live, and help you apply it to your own body.
If you’re ready to move from piecing things together on your own to having a clear, structured path, you can learn more and secure your place here:
https://academy.thefibroguy.com/hypermobility-live-workshop

FAQ on EDS and Diet
Caffeine affects people with EDS differently, but it often worsens common symptoms. It’s a diuretic, which can contribute to dehydration, especially problematic for those with POTS. It may also trigger digestive issues, energy crashes, blood vessel constriction, and histamine intolerance, all of which can exacerbate EDS symptoms. While some tolerate caffeine well, others experience palpitations, shakiness, or fatigue. If you suspect caffeine is affecting you negatively, try reducing or eliminating it and monitor changes. Staying hydrated and consulting a healthcare professional can help manage symptoms.
People with EDS often have deficiencies in vitamin D, B12, magnesium, iron, folate (B9), and vitamin C due to malabsorption, increased nutrient demands, and dietary restrictions. These deficiencies can worsen symptoms like fatigue, pain, muscle cramps, and brain fog. Boosting intake through nutrient-dense foods (leafy greens, fortified cereals, fatty fish, and iron-rich foods) and supplementation when necessary can help manage symptoms and improve overall well-being.
Yes, eggs can be a great addition to the diet for people with EDS. They provide high-quality protein for tissue repair, vitamin D for bone health, and choline for brain function. Eggs also contain antioxidants like lutein and zeaxanthin, which help reduce inflammation, important for managing joint pain and fatigue. Some people with EDS have food sensitivities, so it’s always worth paying attention to how your body reacts. But overall, eggs are a nutrient-dense food that can support connective tissue health when included in a balanced diet.
No, people with EDS don’t necessarily need more protein than the general population, however, getting enough protein is crucial for muscle health, tissue repair, and bone density. Many people with EDS struggle with digestive issues, which can make it harder to meet daily protein needs, leading to fatigue and joint instability. While extra protein or collagen supplements don’t directly improve EDS symptoms, including high-protein foods like eggs, lean meats, fish, dairy, and legumes can support overall health. If eating enough protein is a challenge, protein shakes or supplements may help fill the gaps.
References:
- Choudhary, A., Fikree, A. and Aziz, Q. (2021). Overlap between irritable bowel syndrome and hypermobile Ehlers–Danlos syndrome: An unexplored clinical phenotype? American Journal of Medical Genetics Part C: Seminars in Medical Genetics, 187(4), pp.561–569. doi:https://doi.org/10.1002/ajmg.c.31938.
- Lam, C.Y., Palsson, O.S., Whitehead, W.E., Sperber, A.D., Tornblom, H., Simren, M. and Aziz, I. (2020). Rome IV Functional Gastrointestinal Disorders and Health Impairment in Subjects With Hypermobility Spectrum Disorders or Hypermobile Ehlers-Danlos Syndrome. Clinical Gastroenterology and Hepatology. doi:https://doi.org/10.1016/j.cgh.2020.02.034.
- Alomari, M., Hitawala, A., Chadalavada, P., Covut, F., Al Momani, L., Khazaaleh, S., Gosai, F., Al Ashi, S., Abushahin, A. and Schneider, A. (2020). Prevalence and Predictors of Gastrointestinal Dysmotility in Patients with Hypermobile Ehlers-Danlos Syndrome: A Tertiary Care Center Experience. Cureus. doi:https://doi.org/10.7759/cureus.7881.
- Carbone, F., Fikree, A., Aziz, Q. and Tack, J. (2020). Joint Hypermobility Syndrome in Patients With Functional Dyspepsia. Clinical and Translational Gastroenterology, 11(11), p.e00220. doi:https://doi.org/10.14309/ctg.0000000000000220.
- Correction. (2005). Circulation, 111(13), pp.1717–1717. doi:https://doi.org/10.1161/01.cir.0000163621.17775.a8.
- Zha, K., Brook, J., McLaughlin, A. and Blitshteyn, S. (2022). Gluten-free diet in postural orthostatic tachycardia syndrome (POTS). Chronic Illness, p.174239532210769. doi:https://doi.org/10.1177/17423953221076984.
- Z’Graggen, W.J., Hess, C.W. and Humm, A.M. (2010). Acute fluid ingestion in the treatment of orthostatic intolerance – important implications for daily practice. European Journal of Neurology, 17(11), pp.1370–1376. doi:https://doi.org/10.1111/j.1468-1331.2010.03030.x.
- NHS (2023). Salt in your diet. [online] nhs.uk. Available at: https://www.nhs.uk/live-well/eat-well/food-types/salt-in-your-diet/.
- Bellini, M., Tonarelli, S., Nagy, A.G., Pancetti, A., Costa, F., Ricchiuti, A., de Bortoli, N., Mosca, M., Marchi, S. and Rossi, A. (2020). Low FODMAP Diet: Evidence, Doubts, and Hopes. Nutrients, [online] 12(1), p.148. doi:https://doi.org/10.3390/nu12010148.
- Fragkos, K.C., Keetarut, K., Cox, A., Eady, J., Emmanuel, A.V. and Zarate-Lopez, N. (2019). Joint Hypermobility Syndrome Affects Response to a Low Fermentable Oligosaccharide, Disaccharide, Monosaccharide and Polyol Diet in Irritable Bowel Syndrome Patients: A Retrospective Study. Gastroenterology Research, 12(1), pp.27–36. doi:https://doi.org/10.14740/gr1133.
- Whelan, K., Martin, L.D., Staudacher, H.M. and Lomer, M.C.E. (2018). The low FODMAP diet in the management of irritable bowel syndrome: an evidence-based review of FODMAP restriction, reintroduction and personalisation in clinical practice. Journal of Human Nutrition and Dietetics, 31(2), pp.239–255. doi:https://doi.org/10.1111/jhn.12530.
- Goyal, O., Batta, S., Nohria, S., Kishore, H., Goyal, P., Sehgal, R. and Sood, A. (2021). Low fermentable oligosaccharide, disaccharide, monosaccharide, and polyol diet in patients with diarrhea‐predominant irritable bowel syndrome: A prospective, randomized trial. Journal of Gastroenterology and Hepatology, 36(8), pp.2107–2115. doi:https://doi.org/10.1111/jgh.15410.
- www.ibsdiets.org. (n.d.). FODMAP Food List | IBS Diets. [online] Available at: https://www.ibsdiets.org/fodmap-diet/fodmap-food-list/.
- Munipalli, B., Strothers, S., Rivera, F., Malavet, P., Mitri, G., Dabrh, A.M.A. and Dawson, N.L. (2022). Association of Vitamin B12, Vitamin D, and Thyroid-Stimulating Hormone With Fatigue and Neurologic Symptoms in Patients With Fibromyalgia. Mayo Clinic Proceedings: Innovations, Quality & Outcomes, [online] 6(4), pp.381–387. doi:https://doi.org/10.1016/j.mayocpiqo.2022.06.003.
- Markun, S., Gravestock, I., Jäger, L., Rosemann, T., Pichierri, G. and Burgstaller, J.M. (2021). Effects of Vitamin B12 Supplementation on Cognitive Function, Depressive Symptoms, and Fatigue: A Systematic Review, Meta-Analysis, and Meta-Regression. Nutrients, 13(3), p.923. doi:https://doi.org/10.3390/nu13030923.
- Basalom, S. and Rauch, F. (2020). Bone Disease in Patients with Ehlers–Danlos Syndromes. Current Osteoporosis Reports, 18(2), pp.95–102. doi:https://doi.org/10.1007/s11914-020-00568-5.