This article is part of our comprehensive guide to hypermobility and Ehlers-Danlos syndrome.
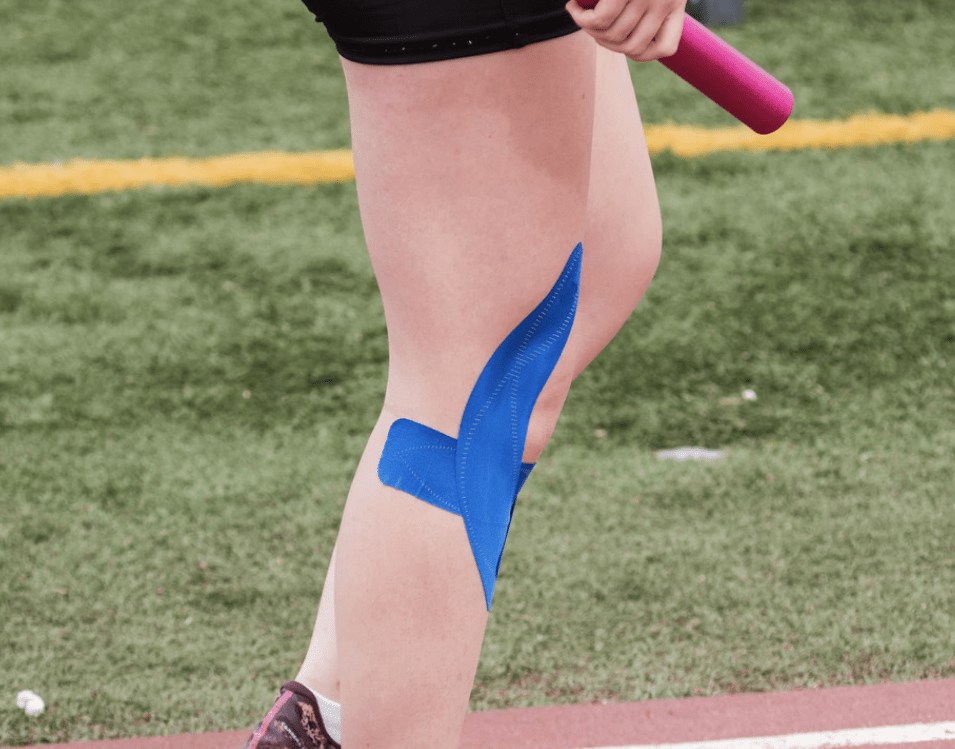
It’s not uncommon to see those with hypermobility and EDS covered in an abundance of brightly coloured tape. At any chronic illness support group, any physiotherapy waiting room, any sports club with a sizeable hypermobile membership, you’ll spot it. Shoulders, knees, wrists, thumbs, ankles. Sometimes all five at once. KT tape has become a kind of unofficial uniform for those of us who sublux regularly and are looking for anything that helps.
And that’s completely understandable. When you’re dealing with joints that feel unreliable, when conventional medical advice has often let you down, and when tape is cheap, available, and doesn’t require a prescription, it’s a pretty appealing option. So this article is going to do something a bit more useful than just listing the marketing claims. We’re going to look at what the evidence actually says, correct a few things that were wrong in our original article on this topic, and bring in four years of new research that changes the picture in some genuinely important ways.
We’ll cover the history, the evidence for and against, what’s happened with the research in hEDS specifically, the proprioception question (which has a new and rather surprising answer), skin reactions (which matter a lot for this population), and some practical tips. There’s a lot to get through, so let’s go.
This article covers:
ToggleA short history of KT tape
Kinesio taping was first developed by chiropractor Kenzo Kase back in the mid-1970s, when he created the tape as a way to support healing after treatment. Much like the ongoing debate around running with hypermobility, the question of whether tape helps or hinders has attracted strong opinions on both sides. It’s worth noting, though, that the name “kinesiology tape” isn’t really about kinesiology as a science. It was a marketing decision. It could have been called anything.
In 1980, Kase established the Kase Chiropractic Clinic in Tokyo and officially trademarked the Kinesio Taping method. By 1985 a dedicated instructor training programme had been developed, and by 1989 the Japanese national volleyball team was using it regularly, which kicked off its international profile. But the real explosion happened at the 2008 Beijing Olympics. Kinesio donated 50,000 rolls to 58 countries, athletes like beach volleyball’s Kerri Walsh were spotted on camera plastered in brightly coloured tape, and the company’s online sales tripled. From that point on, the consumer market went a bit wild. New brands appeared almost overnight, all using the same basic idea. The global sports medicine accessory market is enormous, and when it comes to any shiny new product in that space, it can be hard not to get swept along by the excitement of it all.
The marketing claims and the legal reality
When it comes to the claims made about KT tape, there are quite a few. They vary depending on which brand or website you’re looking at, but here’s a flavour of what gets said:
- Lifts the skin and decompresses the layers of fascia, allowing greater movement of lymphatic fluid
- Promotes the body’s natural healing processes
- Rehabilitation for oedema and swelling management
- Improvement of performance, rehabilitation of neurologic dysfunction, management of scars and posture
- Provides 24-hour pain relief per application
- Recovery, performance, injury prevention
- Supports and stabilises muscles, tendons, and ligaments
Bold claims require extraordinary evidence. And once you cut through the packaging, the brightly coloured tape, and the athlete endorsements, those claims don’t hold up particularly well.
The market eventually caught up with the marketing. Under the terms of the settlement in Vuckovic v. KT Health Holdings Inc. (Case No. 1:15-cv-13696, D. Mass.), KT Health Holdings paid $1.75 million to resolve deceptive marketing allegations. The case centred on claims that the tape could “keep you pain free,” “prevent injury,” and “provide 24-hour pain relief per application.” In addition to creating the settlement fund, KT Health agreed to stop using certain marketing language, and the packaging now includes a bold disclaimer stating the product has not been proven to cure, treat, or prevent any disease or condition.
Likewise, RockTape faced similar class action allegations that its tape doesn’t provide the advertised pain relief. It’s a reminder that sports medicine accessories are a huge business, and the evidence doesn’t always catch up as fast as the marketing does.
What does the evidence actually say?
With so many claims floating around, separating fact from placebo from genuine effect is genuinely difficult. And for those with hypermobility, there’s an added complication: when it comes to the research, a lot of it simply didn’t study hypermobile people at all. That has started to change, which is the main reason this article needed a significant update.
The general KT tape picture
Starting with the broad evidence base: a systematic review published in the Journal of Physiotherapy looked at 12 randomised controlled trials covering shoulder, knee, neck, back, and plantar fasciitis conditions [2]. And the finding was pretty unambiguous. Regardless of what comparison group was used, whether that was sham taping, no treatment, exercises, or conventional physiotherapy, most research showed no significant benefits of KT tape. The review’s conclusion was blunt: “current evidence does not support the use of Kinesio Taping in clinical practice.” It’s worth noting this was a systematic review rather than a meta-analysis, because the included studies were too different from each other to pool the numbers. However, the direction of the evidence was consistent.
When it comes to muscle strength and lower limb performance specifically, a meta-analysis of 37 randomised controlled trials found a more nuanced picture [1]. KT tape did show moderate effects on lower limb muscle strength in people with muscle fatigue and in people with chronic musculoskeletal conditions. However, the same analysis found no significant effect in people without disabilities, and the authors explicitly recommended against the use of KT in that group. So the effects, where they exist, appear to be in clinical populations, not healthy ones. This is worth bearing in mind when we get to the hypermobility-specific evidence.
KT tape and pain
Pain is where the evidence gets a little more interesting. A comparison study in patients with anterior knee pain found that both KT and McConnell taping produced small reductions in pain during stair climbing, though the effect sizes were below the threshold of clinical importance and the study had a very small sample (n=20) [8]. When it comes to low back pain specifically, an RCT published in Chiropractic and Manual Therapies looked at KT tape for chronic non-specific low back pain [4]. The researchers found that KT tape significantly reduced pain and disability scores compared to placebo taping. So something real seemed to be happening for pain. However, and this is important, the same study found no significant improvement in lumbar proprioception (joint position sense in the lower back). We’ll come back to the proprioception question shortly, but for now the point is that KT tape’s effects on pain and its effects on proprioception appear to be separate, and not everything it’s credited with doing is actually happening.
A more rigorous RCT, published in Sports Health, looked at whether adding KT tape to a 10-session physiotherapy programme for rotator cuff-related shoulder pain led to better outcomes than the programme alone [14]. The answer was no. Both groups improved, but there were no significant differences between the KT group and the no-KT group for any outcome, including pain, function, and range of motion. The paper’s own conclusion was clear: “the addition of KT did not lead to superior outcomes compared with exercise-based treatment alone.” This is worth flagging because an earlier version of this blog incorrectly described that study as showing KT was superior to sham treatment. It wasn’t. Both groups improved on the same programme. The tape added nothing.
Dancers, hypermobility, and a corrected statistic
When it comes to hypermobility and dance, there’s been some loose use of statistics in this space, and we want to correct one that appeared in our original article. A literature review (not an original study) by Berezutsky looked at the possibilities of KT tape in preventing injuries in professional dancers with joint hypermobility [6]. Note: these were professional dancers, not recreational ones, which matters because professional dancers have undergone years of intensive training that tends to select for and exacerbate hypermobility. The review concluded that KT tape could reduce muscle spasms, support injured extremities, and ease pain, drawing on published research from 2015 to 2017.
Separately, a cross-sectional study of 77 jazz dancers from the Polish Dance Theater found a significant prevalence of joint hypermobility syndrome in that population [7]. Depending on the diagnostic criteria used, the figures ranged from 59.7% to 74%. Our original article said “up to 95%.” That figure does not appear in the paper. The highest figure the study reports is 74%, via the Hakim and Grahame questionnaire. When it comes to accurate reporting of evidence, that matters. We apologise for that error and have corrected it here.
The first proper EDS-specific evidence (and why it matters that it arrived late)
Here’s the honest truth about where the research stood when we first wrote about this topic. When it comes to EDS-specific data, the only thing available was a two-page conference abstract by Levine and colleagues, published in 2021 in the Archives of Physical Medicine and Rehabilitation [18]. Eight participants. No control group. Short-term follow-up only. It was pilot-level data at best, and citing it as meaningful evidence was always a stretch, even if the direction of the finding was encouraging.
The good news is that the same research group followed that up with something substantially better. In 2023, Levine, Tudini, and colleagues published the first full randomised controlled trial specifically in people with hypermobile Ehlers-Danlos syndrome [9]. Twenty-nine participants (28 female, one male; mean age 41 years) with hEDS and bilateral shoulder pain were randomised to receive either an experimental taping technique that crossed the glenohumeral joint or a control taping technique that did not. Both groups wore the tape for 48 hours.
The results showed that both groups improved significantly in pain and function across multiple validated outcome measures, including the SPADI, QuickDASH, and WOSI questionnaires. Effect sizes were large, particularly for the WOSI (a sport-related shoulder questionnaire). But here’s the catch: there was no significant difference between the two taping groups, and there was no no-tape control arm. We can’t tell whether both groups improved because of the tape, because of the apprehension test used in the study protocol, because of time, because of placebo, or because of some combination of all of these. A 2024 systematic review on conservative interventions for hEDS shoulder confirmed this was the only KT study in this population, and it noted the follow-up was simply too short for conclusive findings [13].
So the picture in hEDS is: something probably happens when you tape a hypermobile shoulder. Both groups improved by amounts that exceeded the minimum clinically important difference on several measures. But we genuinely don’t know what’s driving that, and we only have 48-hour data. That’s meaningful but limited.
KT tape and proprioception: the part where the story changes
This is the section that changed most significantly between our original article and this update. Because the traditional explanation for why KT tape helps those with hypermobility, the one you’ll see repeated across the internet, is that it improves proprioception. That it helps the brain know where the joint is. And it turns out the evidence for that specific claim is far weaker than we thought.
Let’s start with what we already knew. Studies on ankle proprioception found that KT tape had no significant effect on joint position sense in healthy adults [3]. A double-blinded RCT on non-specific chronic low back pain found no significant improvement in lumbar proprioception with KT tape versus placebo [4]. Park and Lee’s 2016 study found interesting differences in walking deviation in stroke patients with hemiplegia who used KT taping [5], but that population and that outcome aren’t directly transferable to hypermobility.
Then in 2023 and 2024, two things happened that changed the picture considerably. First, a large systematic review and meta-analysis by Ghai, Ghai and Narciss pooled data from 91 studies involving 2,718 participants and found that taping does improve joint position sense overall, both compared to no tape and compared to placebo tape [11]. The effect size versus placebo was actually large (Hedges’ g = 1.20), which is notable because it suggests the effect isn’t just a time effect. However, and this is the important caveat, not a single one of those 91 studies was conducted in a hypermobile population. So we have strong evidence that taping improves proprioception in non-hypermobile populations, and essentially no evidence about what it does in people with hypermobility.
Second, a separate systematic review specifically on KT tape and shoulder proprioception found conflicting evidence in healthy populations and very low certainty of any effect in pathological populations like rotator cuff tendinopathy and subacromial pain syndrome [12]. The evidence quality was graded as “very low to low” across all conditions. Mixed findings, small samples, and no consistent taping protocols make drawing firm conclusions impossible. However, the direction of travel is fairly clear: nobody is finding strong, consistent proprioceptive benefits.
But the most important finding came from the companion paper to the Levine 2023 trial. In 2024, Tudini and colleagues published an RCT using the same 29-participant hEDS cohort, this time examining shoulder range of motion and, crucially, active joint repositioning (a standard proprioception test) [10]. The researchers compared the GH-crossing taping technique with the non-crossing control technique in hEDS participants.
The range of motion finding was interesting: the GH-crossing tape significantly improved external and internal rotation in the shoulder, while the non-crossing tape did not. That’s a genuinely useful finding, because it suggests the mechanical direction of the tape matters, at least for range of motion.
But for proprioception? No significant improvement in active joint repositioning was found in either group. The interaction effect was non-significant (p=0.19). This is the first and currently only study to test KT tape proprioception in a population with hEDS, and it found no effect. In fact, the control group showed a trend toward worsening proprioception at 48 hours, though that also wasn’t statistically significant.
A 2025 RCT on shoulder instability patients (not hEDS specifically, but glenohumeral instability, which is highly relevant) found a similar dissociation [16]: KT tape did not improve proprioception as measured by electronic goniometry, but it did improve perceived joint stability and patient-reported function. A separate systematic review and meta-analysis looking at KT tape in athletes with chronic ankle instability also found significant effects on gait function and a significant reduction in medial-lateral sway velocity, without significant effects on dynamic balance or other postural sway measures [17]. So across different joints and populations, the theme is consistent: KT tape affects movement and perceived stability in ways that don’t always show up on standard proprioception tests. Something is happening. It just doesn’t appear to be proprioception as we usually measure it.
So the mechanism most commonly cited for KT tape in EDS, that it improves proprioception, doesn’t appear to be supported by the evidence we now have. The tape may do something neuromuscular, something related to skin mechanoreceptors, or something attentional, but the idea that it’s restoring accurate joint position sense is not currently backed up by data. This is worth sitting with, because when it comes to explaining why tape helps, many clinicians and patients have leaned heavily on the proprioception story. That story needs revising.
Why might KT tape still help with pain?
Well, here’s where it gets interesting. Because even if proprioception isn’t the mechanism, people with hypermobility do report meaningful benefit from tape. And the research (however limited) shows that something is happening in hEDS. So what’s going on?
For those with hypermobility and EDS, and especially for those who sublux or partially dislocate joints regularly, nociceptive pain is a significant feature. Nociception is where high-threshold nerve endings detect potentially damaging stimuli, including extreme stretch of soft tissue, and relay that information to the brain. The mechanisms behind chronic pain in hypermobility are more complex than this, but let’s use a simple example.
Say you partially sublux your hypermobile ankle. The extreme stretching of ligaments and tendons, something worth reading about more if stretching and hypermobility is a topic you haven’t explored yet, is likely to trigger a nociceptive response. Your nervous system goes on high alert. Local inflammation follows. And because of this heightened sensitivity, even inputs you’d normally ignore, like your sock touching your skin, now get flagged and sent upward to the brain.
Tape almost certainly acts as a competing input in that context. When it comes to pain modulation, the continuous tactile stimulation the tape provides is picked up by the same sensory pathways that carry nociceptive information. In effect, it crowds out some of the alarm signals with something less threatening. This is broadly consistent with gate control theory, the idea that non-nociceptive sensory input can modulate the transmission of pain signals in the spinal cord. We’re also humans, and we’re incredibly tactile creatures from birth. Touch is one of the first things we reach for when something hurts, it’s instinctive, and there’s a reason for that.
It’s also worth noting that pain in hEDS often has a nociplastic component, meaning there’s central sensitisation involved. For that kind of pain, peripheral sensory input from tape may be less effective as a standalone intervention. However, it can still contribute to a broader picture of comfort and body awareness, and there’s something to be said for any intervention that reduces the sense of threat around a joint that feels chronically unreliable. We’re not claiming the tape is doing what the packaging says. We’re saying the mechanism that probably is operating is sensory modulation, not structural support, not lymphatic drainage, and not, as far as we can tell, proprioception.
If you want to understand more about how the nervous system processes pain in conditions like this, our courses on chronic pain and hypermobility go into considerably more depth on the underlying mechanisms.
KT tape doesn’t immobilise joints, and that’s genuinely good news
One of the stronger arguments for KT tape in hypermobility, and one that holds up well, is that it doesn’t immobilise. This sounds like damning with faint praise, but it’s actually important.
Immobilisation of a joint that’s repeatedly subluxing is a very understandable response. If the joint keeps going out, the instinct is to stop it moving. However, the consequences of prolonged immobilisation for those with EDS are significant. Hypoxic and inflammatory conditions can develop in the joint capsule. Articular cartilage can become thinner. Collagen content increases as the body lays down what’s essentially scar tissue. When it comes to joint health, research has shown that immobilised cartilage is structurally inferior to cartilage in an appropriately loaded joint, the trabecular bone plate area decreases, and in some cases irregular repair processes begin where bone starts replacing cartilage. These are real clinical concerns, particularly for joints that are already structurally compromised in conditions like hEDS.
Equally, the evidence is well-established that loading a joint appropriately, through movement and progressive exercise, strengthens bone and supports cartilage health. We’ve written about this extensively in relation to exercise and hypermobility. There are also implications here for specific areas like rib subluxations and scoliosis in hypermobility, where immobilisation can set off a similar cascade of problems. When it comes to joint stability in hypermobility, the goal is not to protect the joint by stopping it moving. It’s to stabilise it through building the muscular and neuromuscular control that supports it during movement.
KT tape occupies a sensible middle ground here. It provides some sensory input, some sense of support, and doesn’t prevent the full range of movement needed for that neuromuscular training to happen. Rigid bracing is a different matter, and in many cases a worse option for joints that need loading. KT tape, by contrast, moves with you. Now, that doesn’t make it the whole answer. But it does mean it’s a reasonably sensible tool to use alongside a proper rehabilitation programme.
Skin reactions and MCAS: a section the original article didn’t have
This is new territory for this blog post, and honestly it’s the section I wish we’d included the first time around. Because for a significant chunk of people with hEDS, particularly those who also have mast cell activation syndrome (MCAS), skin reactions to KT tape are a real and sometimes serious problem.
EDS comes with skin that is often more fragile, more extensible, and more reactive than average. What causes a minor irritation in someone without connective tissue disease can cause a meaningful reaction in someone with hEDS. And when you layer MCAS on top of that, the sensitivity increases further, because MCAS involves dysregulated mast cell activation that can generate heightened responses to chemical and physical triggers, including adhesives. When it comes to tape adhesives specifically, the relevant chemistry matters more than most people realise.
The colophonium problem
A 2023 investigation of an outbreak of contact dermatitis in 26 military conscripts who wore medical adhesive tape continuously during a field exercise found that 61% had confirmed colophonium allergy [15]. Colophonium (also called rosin or colophony) is a pine-resin derivative used as a tackifier in many medical adhesives, including kinesiology tape. What was striking about the Hamnerius et al. study wasn’t just the percentage, it was that most of these individuals had no prior history of colophonium exposure. The tape itself appeared to be inducing the sensitisation. And once you’re sensitised to an allergen, repeat exposure reliably triggers a reaction.
Colophonium allergy is not rare in the broader tape-using population either. Data from North American Contact Dermatitis Group patch-testing (43,722 patients, 2001-2018) identified colophony as the most common allergen in medical adhesive contact allergy, accounting for over 80% of positive reactions in relevant cases. If you’re reacting to KT tape, this is probably why.
Other relevant allergens in tape adhesives include acrylates, zinc oxide, and rubber-related additives. However, the community consensus across multiple EDS forums and subreddits is that RockTape produces fewer reactions than standard KT Tape brand, with community members attributing this to RockTape lacking zinc oxide. There’s no published comparative allergen testing to confirm this, but it’s consistent enough across patient experience reports to be worth noting.
MCAS and tape reactions
There is no published clinical study on KT tape reactions specifically in people with MCAS or EDS. That’s a significant evidence gap, and it’s one that the patient community has essentially been filling on its own. What we know from the patient community is that MCAS-associated tape reactions can go beyond local skin irritation. There are reports of systemic reactions, including hives, nausea, and histamine-type responses that go beyond what you’d expect from a simple contact allergy. The Levine and Tudini 2023-2024 studies reported a 5.2% rate of minor skin reactions (redness, blistering) in their hEDS sample, and none of the enrolled participants were documented as having MCAS. The real rate in an hEDS and MCAS population is likely higher, possibly considerably so.
If MCAS is something you’re managing alongside your hypermobility, our guide to MCAS covers the broader picture. A few practical approaches have been reported in the EDS community and are worth knowing about, even in the absence of clinical trials.
Types of skin reaction
Broadly speaking, there are four types of reaction worth distinguishing. First, there’s irritant contact dermatitis, which is mechanical irritation from the adhesive, worsened by heat, friction, and repeated application. Second, there’s allergic contact dermatitis, a Type IV delayed hypersensitivity reaction, typically appearing 24 to 96 hours after application, driven by allergens like colophonium. Third, there are MCAS-mediated reactions, which can be immediate or delayed and may involve systemic symptoms beyond the skin. Fourth, there’s mechanical skin damage from forcible removal, which can cause skin tears in EDS, where skin fragility is already a feature. When it comes to removal, dry-pulling is something to avoid entirely. Water, oil, or adhesive remover products are always safer.
Practical tips for taping when you’re hypermobile
So, assuming you want to try tape or you’re already using it, here’s what actually makes a difference in practice.
Sensitive skin and barrier techniques
If you have reactive skin, or if you’ve had reactions before, applying a barrier between your skin and the tape is worth trying. Options used by people in the EDS community include dedicated skin barrier sprays (the type used in stoma care), barrier wipes, or applying Milk of Magnesia to the area and letting it dry first. Some patients whose skin reactions are severe enough have had a specialist prescribe a fluticasone inhaler spray to apply to the skin before taping. This provides a mild topical corticosteroid effect that can prevent the reaction without reducing tape adhesion. That’s not something to try on your own initiative without medical guidance, but it illustrates that solutions exist for those who need tape and also react to it.
If you regularly react to one brand, try a different one. RockTape has a strong reputation within the EDS community for being better tolerated, particularly for those with adhesive sensitivity or MCAS. However, whether that’s genuinely down to the adhesive composition or something else isn’t confirmed by published research. The community consensus is consistent enough to be worth trying.
Shave the area first
Trust us on this one. Removing KT tape from a hairy area is not pleasant and carries its own risk of skin damage in EDS. If you’re going to tape a joint, shave the area beforehand. Your future self will thank you.
Remember that the tape stretches
Most quality KT tape stretches up to 140% of its original length. People frequently cut far more tape than they need. Start with less than you think you need, because you can always add more, and the tape itself can do more work than a longer piece applied without stretch.
Round off the ends
KT tape has a persistent tendency for the corners of the ends to curl up, which then snags on clothing and often pulls the tape off prematurely. Cut the ends into a rounded shape before application. It makes a meaningful difference to how long the tape stays put.
Tear the backing paper
If you try to peel the backing paper off from one end, you’ll often struggle, especially if you have wrist pain or hypermobility in your hands. Instead, tear the backing paper across the width of the tape in the centre, then peel outward from that tear in both directions. Much easier.
Remove in the shower or bath
When it’s time to take the tape off, do it in the shower or bath, after the tape has been wet for at least a few minutes. It comes off significantly more easily, causes less skin irritation, and dramatically reduces the risk of mechanical skin damage from forcible dry removal. If you have MCAS or fragile skin, oil-based removal products (baby oil, mineral oil, jojoba oil) used in water or directly onto dry tape are also excellent. If your tape is fighting you, stop and get it wet first.
A word about the neck
Patient community reports have flagged a concern that’s worth mentioning: some people with hEDS who have taped their neck or upper cervical region have reported worsening of cervical instability symptoms. The proposed mechanism is that tape applied to relax overactive paraspinal muscles may over-relax stabilising muscles in a region that already has compromised structural support. There’s no formal study on this, but it’s mechanistically plausible and clinically important. If you have cervicogenic symptoms, coat hanger pain, or any concerns about cranio-cervical instability, be cautious about cervical taping and discuss it with an EDS-literate clinician first.
Should you use KT tape for hypermobility and EDS?
Right, so let’s try to pull this together into something actually useful.
Something happens when you tape a hypermobile joint. We’ve now got enough evidence to say that with reasonable confidence. The Levine 2023 RCT in hEDS showed large effect sizes for pain and function in a real hEDS sample [9]. The mechanism most commonly invoked, improved proprioception, isn’t supported by the data we now have, but range of motion appears to respond to tape that crosses the glenohumeral joint, and sensory modulation via tactile input remains a plausible explanation for the pain effects [10].
What we still don’t know is whether those effects persist beyond 48 hours, whether they’re specific to taping or would occur with any well-applied adhesive, and whether the improvements reflect genuine neuromuscular benefit or something closer to a time and attention effect. The absence of a no-tape control group in both EDS-specific RCTs means we can’t answer that question from the current data. When it comes to technique, it’s also genuinely interesting to note that both taping approaches in Levine 2023 worked equally well, which suggests the specific method matters less than people often assume.
Here’s where we stand on the individual claims. And it’s worth being direct about this, rather than hedging everything into meaninglessness.
Does KT tape provide structural support and prevent subluxations? Not in any meaningful mechanical sense. The elastic properties of the tape aren’t strong enough to prevent joint movement, which is actually the point. It moves with you.
Does it improve proprioception? Based on the best available evidence in hEDS, which is currently one RCT, the answer appears to be no, at least not as measured by active joint repositioning. This is a significant revision from what has been claimed both in this blog and across the field.
Does it help with pain? There’s reasonable evidence that it does something for pain, both in the general population and in the specific hEDS RCT. Whether that’s tactile modulation, placebo, or something else, the effect appears real in a proportion of people.
Is it dangerous? Generally not, but skin reactions are a real risk in EDS, particularly in those with MCAS. Knowing how to apply and remove tape correctly reduces that risk considerably.
Does it immobilise? No. And that’s genuinely one of its better features.
So the honest answer to the question of whether you should use KT tape is: if it helps you, use it, but don’t rely on it as your primary strategy. When it comes to managing hypermobility long-term, tape is at best a piece of the puzzle, not the whole picture. Poor sleep, anxiety, and general deconditioning all interact with joint stability in ways that tape can’t address. Tape doesn’t build the neuromuscular control that stabilises hypermobile joints over the long term. That comes from progressive, well-structured exercise, from building strength and proprioceptive confidence in the muscles that support your joints. Some of our clients’ results demonstrate what that kind of rehabilitation can achieve. You can read more about approaches to specific areas including hypermobile knees, flat feet, shoulder stability, elbows, and tibial rotation throughout our site.
Tape can be a useful adjunct, particularly during EDS flares, during activities that put extra demand on a joint, or while you’re building the strength that will eventually make you less reliant on it. But it isn’t the solution. It’s a tool in a toolkit, and it’s important to keep it in that context. For those navigating the full picture of how to manage hypermobility symptoms, including approaches to pacing, and the fear of movement that often develops alongside chronic instability, the broader picture matters at least as much as any single intervention.
If you’re looking to take things a step further, our online courses or one-to-one consultations offer structured guidance built specifically for those with hypermobility and EDS. And if you haven’t already explored the full symptom picture of hypermobility spectrum disorders, that’s also worth doing to get a clearer sense of everything you’re working with.
We hope this updated version is genuinely more useful than the original. It’s a better article because the evidence is better. Four years of research, two actual EDS-specific RCTs, and a major meta-analysis on proprioception have changed what we can responsibly say about this topic. When it comes to KT tape and hypermobility, the picture is clearer than it was, even if some of the certainty we’d like still isn’t there yet.
– The Fibro Guy Team –
How to tape hypermobile joints
Below are two videos demonstrating KT tape application for specific hypermobile joints. The shoulder video is particularly relevant given the research discussed above.
How to KT tape a hypermobile wrist and thumb
For those with wrist pain and hypermobility, or hypermobility at the thumb, taping can help provide that tactile feedback during activities that demand grip or fine motor control.
How to tape a hypermobile shoulder
Given the Levine 2023 and Tudini 2024 findings on GH-crossing tape for shoulder range of motion, the technique used matters more than you might think. This video walks through the application for a hypermobile shoulder.
References
- Yam, M.L., Yang, Z., Zee, B.C.-Y. and Chong, K.C. (2019). Effects of Kinesio tape on lower limb muscle strength, hop test, and vertical jump performances: a meta-analysis. BMC Musculoskeletal Disorders, 20(1). doi: 10.1186/s12891-019-2564-6
- Parreira, P. do C.S., Costa, L. da C.M., Hespanhol Junior, L.C., Lopes, A.D. and Costa, L.O.P. (2014). Current evidence does not support the use of Kinesio Taping in clinical practice: a systematic review. Journal of Physiotherapy, 60(1), pp.31-39. doi: 10.1016/j.jphys.2013.12.008
- Halseth, T., McChesney, J.W., DeBeliso, M., Vaughn, R. and Lien, J. (2004). The Effects of Kinesio™ Taping on Proprioception at the Ankle. Journal of Sports Science and Medicine, 3(1), pp.1-7. Available at: https://pmc.ncbi.nlm.nih.gov/articles/PMC3896108/
- Abbasi, S., Hadian Rasanani, M.-R., Ghotbi, N., Olyaei, G.R., Bozorgmehr, A. and Rasouli, O. (2020). The effect of Kinesio taping on postural control in subjects with non-specific chronic low back pain. Chiropractic and Manual Therapies, 28(1). doi: 10.1186/s12998-020-00349-y
- Park, Y.-H. and Lee, J.-H. (2016). Effects of proprioceptive sense-based Kinesio taping on walking imbalance in persons with stroke. Journal of Physical Therapy Science, 28(11), pp.3060-3062. doi: 10.1589/jpts.28.3060
- Berezutsky, V. (2018). Possibilities of kinesio taping to prevent injuries of professional dancers with joint hypermobility. International Journal of Occupational Safety and Ergonomics, 25(4), pp.638-645. doi: 10.1080/10803548.2018.1433281
- Skwiot, M., Śliwiński, G., Milanese, S. and Śliwiński, Z. (2019). Hypermobility of joints in dancers. PLOS ONE, 14(2), p.e0212188. doi: 10.1371/journal.pone.0212188
- Campolo, M., Babu, J., Dmochowska, K., Scariah, S. and Varughese, J. (2013). A comparison of two taping techniques (kinesio and mcconnell) and their effect on anterior knee pain during functional activities. International Journal of Sports Physical Therapy, 8(2), pp.105-110. Available at: https://pubmed.ncbi.nlm.nih.gov/23593548/
- Levine, D., Tudini, F., Chui, K.K., Jordon, M.K. and Healy, M. (2023). Evaluating the effects of two different kinesiology taping techniques on shoulder pain and function in patients with hypermobile Ehlers-Danlos syndrome. Frontiers in Pain Research, 4:1089748. doi: 10.3389/fpain.2023.1089748
- Tudini, F., Jordon, M., Levine, D., Healy, M., Cathey, S. and Chui, K.K. (2024). Evaluating the effects of two different kinesiology taping techniques on shoulder range of motion and proprioception in patients with hypermobile Ehlers-Danlos syndrome: a randomized controlled trial. Frontiers in Rehabilitation Sciences, 5:1383551. doi: 10.3389/fresc.2024.1383551
- Ghai, I., Ghai, S. and Narciss, S. (2024). Influence of taping on joint proprioception: a systematic review with between and within group meta-analysis. BMC Musculoskeletal Disorders, 25:478. doi: 10.1186/s12891-024-07571-2
- Ager, A.L., de Oliveira, F.C.L., Roy, J.S., Borms, D., Deraedt, M., Huyge, M., Deschepper, A. and Cools, A.M. (2023). Effects of elastic kinesiology taping on shoulder proprioception: a systematic review. Brazilian Journal of Physical Therapy, 27(4):100514. doi: 10.1016/j.bjpt.2023.100514
- Higo, A., Liaghat, B., Pearce, G., Tallis, J., Silvester, L. and Palmer, S. (2024). The Effectiveness of Conservative Interventions on Pain, Function, and Quality of Life in Adults with Hypermobile Ehlers-Danlos Syndrome/Hypermobility Spectrum Disorders and Shoulder Symptoms: A Systematic Review. Archives of Rehabilitation Research and Clinical Translation, 6(3):100360. doi: 10.1016/j.arrct.2024.100360
- de Oliveira, F.C.L., Pairot de Fontenay, B., Bouyer, L.J., Desmeules, F. and Roy, J.-S. (2020). Kinesiotaping for the Rehabilitation of Rotator Cuff-Related Shoulder Pain: A Randomized Clinical Trial. Sports Health, 13(2), pp.161-172. doi: 10.1177/1941738120944254
- Hamnerius, N., Dahlin, J., Bruze, M., Nilsson, K. and Sukakul, T. (2023). Colophonium-related Allergic Contact Dermatitis Caused by Medical Adhesive Tape Used to Prevent Skin Lesions in Soldiers. Acta Dermato-Venereologica, 103:adv18428. doi: 10.2340/actadv.v103.18428
- Bręborowicz, E., Olczak, I., Romanowski, L., Bręborowicz, M., Ślęzak, M., Lubiatowski, P. and Ogrodowicz, P. (2025). Using an Electronic Goniometer to Assess the Influence of Single-Application Kinesiology Taping on Unstable Shoulder Proprioception and Function. Sensors, 25(7):2326. doi: 10.3390/s25072326
- Biz, C., Nicoletti, P., Tomasin, M., Bragazzi, N.L., Di Rubbo, G. and Ruggieri, P. (2022). Is Kinesio Taping Effective for Sport Performance and Ankle Function of Athletes with Chronic Ankle Instability (CAI)? A Systematic Review and Meta-Analysis. Medicina, 58(5):620. doi: 10.3390/medicina58050620
- Levine, D., Tudini, F., Healy, M., Dunlap, A., Merritt, M., Vaught, E. and Norman, K. (2021). The Short Term Effects of Kinesiology Taping on Shoulder Pain and Function in Patients with Ehlers-Danlos Syndrome. Archives of Physical Medicine and Rehabilitation, 102(10), pp.e26-e27. doi: 10.1016/j.apmr.2021.07.535